A Clinician's Guide to Online Tests for Dementia
Jan 9, 2026

Online dementia tests are quick, digital tools that screen for the early signs of cognitive change. It's important to remember they are not diagnostic. Think of them like a blood pressure reading for heart health—they're an initial checkpoint to see if a more thorough clinical evaluation is a good idea.
The Shift to Digital Dementia Screening in Healthcare
The way clinicians approach cognitive health is changing. Not long ago, assessing a patient’s memory or thinking skills was a lengthy, specialist-driven process, usually saved for when symptoms were already quite obvious. Now, rapid and accessible online tests for dementia are becoming go-to tools in primary care, giving us a proactive way to monitor brain health.
This shift is born from a simple, pressing need: our population is getting older, and with that, the prevalence of cognitive conditions is on the rise. Clinicians on the front lines need efficient ways to spot potential issues early, long before they become a crisis.
A First Alert for Cognitive Health
It’s helpful to think of these digital assessments as a first-alert system for the brain. They aren't designed to give a definitive diagnosis of Alzheimer's or any other form of dementia. Their real power is in their ability to flag subtle changes in cognitive function that might easily go unnoticed during a routine check-up.
These tools provide objective data points to start a conversation. A concerning result doesn’t mean a diagnosis; it means it’s time for a deeper, more comprehensive clinical investigation.
This initial screening helps make the care pathway much more efficient. By identifying individuals who might be at risk sooner, clinicians can prioritise specialist referrals and start having those important conversations with patients and their families about what to do next.
Why This Matters for Modern Clinicians
Bringing these tools into a practice is a key part of the larger move toward preventative, data-driven medicine. The growth of online dementia tests is a perfect example of the broader trend of digital transformation in the healthcare industry, where technology helps make care more accessible and efficient. For any busy practice, the benefits are clear:
Early Detection: Digital screeners can pick up on slight declines in memory, attention, or executive function that might signal the very earliest stages of cognitive impairment.
Data-Driven Decisions: They replace subjective impressions with objective, measurable data. This is invaluable for tracking cognitive changes over time.
Improved Efficiency: A quick, tablet-based test that a patient can take in the waiting room gathers valuable information without taking up precious time on the physician's schedule.
The sheer scale of the challenge makes these tools more necessary than ever. In California, for example, the Alzheimer’s Association estimates that 720,000 residents aged 65 and older are living with Alzheimer’s dementia. With state projections showing this number could climb past 850,000 by 2025, the need for scalable, initial screening solutions in primary care settings has never been more critical. You can learn more about dementia statistics and its impact in California.
Navigating the Different Types of Online Cognitive Tests
When you start looking into online tests for dementia, it becomes clear pretty quickly that not all digital tools are the same. They run the gamut from simple apps aimed at consumers to highly sophisticated instruments designed for clinical use. The key is knowing which one to reach for, and that decision comes down to the clinical context and what you need to learn about a patient's cognitive health.
Think of it like choosing a tool from a toolbox. You wouldn't use a sledgehammer to fix a pair of glasses. In the same way, the cognitive test you choose has to match the clinical question you're trying to answer, whether that's a routine check-up or a deep dive into specific memory complaints.
This diagram helps visualize where online screening sits within the bigger picture of dementia care.
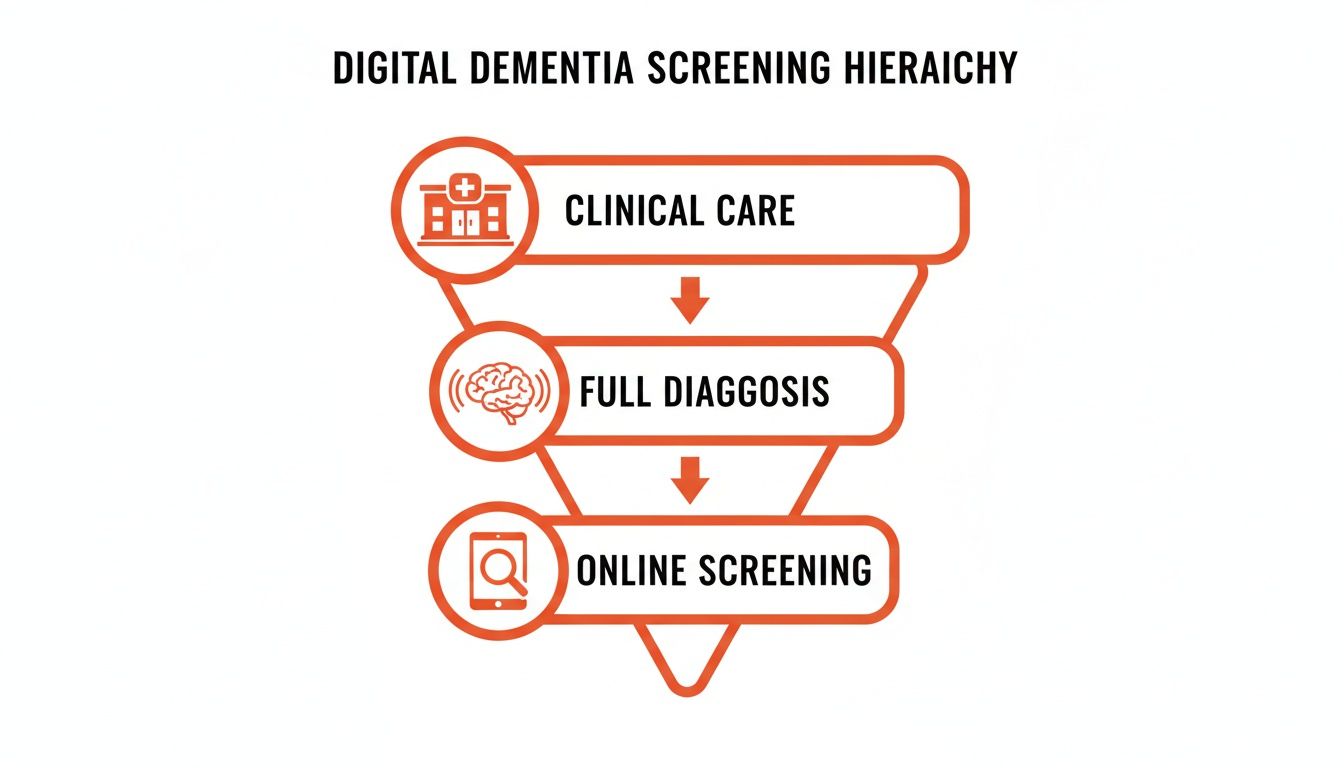
As you can see, online screening is really that first, foundational step. It's built to cast a wide net and help identify individuals who might need a closer look through a full diagnostic workup in a formal clinical setting.
Quick Cognitive Screeners
The most common and straightforward tools are the quick cognitive screeners. These are short, simple tests designed to be a first pass, flagging potential issues without getting bogged down in detail. They are built for speed and accessibility, which makes them perfect for initial triage in busy practices.
For example, a family doctor might use a 5-minute, tablet-based screener during an annual wellness visit for a patient in their 70s. The test could involve recalling a few words or drawing a clock. A low score doesn't mean a diagnosis; it's simply an objective signal that a more thorough assessment is probably a good idea.
Comprehensive Cognitive Batteries
A step up in complexity are the comprehensive cognitive batteries. These are much more detailed digital assessments that probe function across several cognitive domains—things like memory, attention, executive function, and processing speed. They paint a far richer, more nuanced picture of a person’s cognitive profile.
These are the tools you’d turn to after a quick screener raises a red flag. Following that wellness visit, the doctor could have the same 70-year-old patient complete a 20-minute assessment in the clinic. This battery would provide specific data points that help distinguish between normal, age-related forgetfulness and a pattern that looks more like Mild Cognitive Impairment (MCI). You can dive deeper into these kinds of assessments in our guide to finding a quality cognitive screening test online.
These more extensive batteries move beyond a simple "pass/fail." They offer a granular view that can guide what comes next—whether that’s a referral to a specialist or a period of "watchful waiting" with regular re-testing to track any changes.
Digital Biomarker Tools
The newest and most advanced category is digital biomarker tools. You can think of these as a 'Fitbit for the brain.' Instead of a one-off test, these tools often use technology like smartphones or wearables to continuously or frequently monitor subtle behavioural patterns.
A specialist, for instance, might use a tool that passively tracks a patient's typing speed, speech patterns, or even their gait through their phone's sensors over several weeks. A gradual decline in typing accuracy or a shift in vocal tone could act as a digital biomarker, offering real-world data on cognitive function outside the sterile environment of a clinic. This is an incredibly powerful approach for long-term monitoring and catching very subtle changes early on.
To help you decide which tool best fits your clinical workflow, the table below provides a clear, side-by-side comparison of these different formats.
Comparing Online Dementia Test Formats
This table breaks down the primary types of online tests, outlining their purpose, typical use case, and key limitations to help clinicians choose the right tool for the right situation.
Test Type | Primary Purpose | Example Use Case | Key Limitation |
|---|---|---|---|
Quick Screeners | Initial, rapid detection of potential cognitive concerns. | A 5-minute test during a routine annual physical for an older adult. | Lacks detail; high potential for false positives or negatives. |
Cognitive Batteries | Detailed assessment across multiple cognitive domains. | A 20-minute follow-up test after a patient reports memory issues. | Requires more time to administer and interpret than a simple screener. |
Digital Biomarkers | Continuous, long-term monitoring of real-world function. | Passively tracking a patient's typing speed and speech patterns over months. | Still an emerging field; data can be complex to interpret and integrate into EHRs. |
Ultimately, understanding these distinctions is key. It allows you to select an online cognitive test that provides the right level of information for each patient's unique situation, ensuring your clinical decisions are guided by precise, relevant data.
Understanding Validity and Ethical Responsibilities
When you're thinking about bringing online dementia tests into your practice, it's completely normal to have questions about their accuracy and the ethical duties that come with them. Adopting any new tool means taking a hard look at its reliability and how it handles patient data. These aren't just technical checkboxes; they're at the very heart of responsible care.
The path forward is all about balancing the convenience of digital tools with the tough standards we hold in clinical practice. This means getting a real feel for what "clinically validated" actually means in this new context and being honest about the limits of these screeners.

What Clinical Validation Really Means
The term clinically validated is far more than a marketing buzzword—it’s a badge of scientific proof. It signifies that an online test has been put through its paces against traditional, gold-standard neuropsychological assessments (think the MoCA or MMSE) in research studies. It has proven that it measures what it’s supposed to measure, accurately and consistently.
This rigorous process is what separates a reliable clinical instrument from a simple brain game. For a deeper dive into this, our guide on the principles of reliability in test-retest scenarios breaks down exactly how we measure consistency. A truly validated test gives you confidence that the results are a genuine reflection of cognitive function.
But validation isn't a blanket approval for every situation. It’s absolutely vital to understand the limitations of any screening tool, whether it's on a tablet or a piece of paper.
Acknowledging the Limitations Head-On
Let's be clear: even the very best online dementia tests are not diagnostic tools. They’re designed to raise a flag, to signal that something warrants a closer look—not to deliver a final verdict. It's incredibly important to manage these expectations, both for yourself and for your patients.
Here are a few key limitations to always keep in mind:
Screening vs. Diagnosis: Think of a concerning score as the start of a conversation, not the end of one. It’s a sign that a full clinical workup is needed to explore all possibilities and arrive at an accurate diagnosis.
Technological Literacy: How comfortable a patient is with a tablet or computer can absolutely affect their performance. A low score might say more about their unfamiliarity with the tech than it does about their cognitive state.
The Full Clinical Picture: These results have to be placed within the patient's wider health story. Things like medication side effects, poor sleep, chronic pain, or depression can all drag down cognitive scores.
Remember, the score from an online test is just one data point. It gains its true clinical value only when combined with your medical judgment, the patient’s history, and reported symptoms.
Your Ethical Responsibilities: Data Security and Patient Privacy
Beyond clinical accuracy, you have to navigate crucial data privacy regulations like HIPAA compliance to protect sensitive patient information. When you use a digital platform, you're entrusting it with protected health information (PHI), and that comes with serious ethical and legal weight.
Before you bring any online cognitive testing platform into your workflow, run it through this quick checklist:
Clear Privacy Policy: Does the company have a straightforward, easy-to-find privacy policy explaining what data they collect and how they use it?
Data Encryption: Is patient data encrypted both while it's being sent over the internet and while it's sitting on their servers?
Access Controls: Does the platform have strong safeguards to make sure only authorized people can access patient data?
How you talk to patients about this is just as important. Framing the test in the right way can help manage anxiety and set clear expectations. For example, you could say: "We're going to do a quick check-up for your brain health today. This is a screening, much like a hearing test, to get a baseline. It helps us see if there's anything we need to look into more closely."
This simple script positions the test as a routine part of proactive care, not a scary, high-stakes event. It helps build a more collaborative and less stressful experience for everyone involved.
How to Interpret and Act on Screening Results
Getting the results from an online cognitive test is a pivotal moment, but the raw score is really just the opening line of a much deeper conversation. A number by itself doesn't tell you the whole story. Its real value emerges only when you place it into the rich context of a person's life—their medical history, their personal baseline, and the subtle changes they or their family have started to notice.
The trick is to turn that data point into a concrete, actionable care plan. This means moving beyond a simple "pass" or "fail" mindset. Instead, the result should act as a catalyst for a more informed, productive conversation about brain health. The aim is to figure out the most sensible next step, making sure it’s proportional to the result without causing unnecessary alarm.
Creating a Decision-Making Framework
So, you have a test result. The big question is: what does this actually mean for this specific individual? Not every score calls for the same response. A structured approach helps standardise care and ensures every person gets the right level of attention for their unique situation.
Here’s a practical framework for sorting results and planning what comes next:
Reassurance and Lifestyle Guidance: If a patient's score is well within the normal range and they report no concerns, this is your chance to reinforce proactive brain health habits. Actionable step: Provide a simple handout on the pillars of brain health: regular exercise, a Mediterranean-style diet, social engagement, and quality sleep.
Watchful Waiting and Re-testing: For a borderline score with no major functional complaints, a "wait and see" approach is often best. Actionable step: Schedule a follow-up screening in 6 to 12 months and have the patient or their family keep a simple journal of any memory lapses or difficulties with daily tasks.
Further In-Clinic Investigation: A score that lands clearly below the normal range should trigger a deeper look. Actionable step: Order a standard panel of blood tests to check for vitamin B12 deficiency, thyroid issues, and other reversible causes. Conduct a thorough medication review to identify any drugs known to cause cognitive side effects.
Immediate Specialist Referral: A very low score, particularly when paired with reported functional difficulties (e.g., getting lost, trouble managing finances), warrants a prompt referral. Actionable step: Send a referral to a neurologist or memory clinic that includes the screening results, your clinical notes, and relevant patient history.
Discussing Results with Empathy and Clarity
The way you talk about the screening results is just as important as the score itself. This conversation has to be handled with real empathy and care to empower people and their families, not frighten them. The key is to frame the online test as just one piece of a much larger puzzle.
The most productive conversations about cognitive screening results focus on partnership. Frame the score not as a label, but as shared information that helps you and your patient decide together what to do next to protect their brain health.
For example, you might start the conversation like this: "We have the results from your cognitive check-up. This score gives us a useful snapshot of your brain health today. It looks a little lower than we'd expect, which tells me we should look into this a bit more closely together. There are many things that can affect these scores, so our next step will be to explore those."
This approach avoids alarming language and frames the result as a signal for collaborative problem-solving. It’s absolutely crucial for maintaining trust and making sure the person stays engaged in their own care. For anyone wanting more detailed guidance, resources on MoCA score interpretation offer deeper insights into how specific test outcomes connect to clinical decisions.
Initiatives in places like California are already building the infrastructure to make this kind of stepped-care model a reality. The UCSF-led Dementia Care Aware program, for instance, trains primary care teams to embed brief Cognitive Health Assessments into regular visits. This statewide shift shows how rapid, tech-enabled assessments are becoming the new front end of a clear pathway, channelling at-risk individuals toward the comprehensive work-ups they need. You can discover more about California's approach to dementia care and see the impact it's having on public health.
Integrating Digital Screening Into Your Clinical Workflow
Bringing online dementia tests into your practice is about more than just picking a new tool. It’s about thoughtfully weaving it into the very fabric of your daily operations. A smart rollout needs a clear plan, from getting your staff on board to pinpointing exactly when and how patients will take the assessment. The idea is to make cognitive screening a routine part of care, not just an afterthought.
This turns a good idea into a practical, repeatable system. It makes sure every patient gets the same high standard of proactive brain health monitoring, making early detection a systematic process rather than a matter of chance.

Step 1: Select a Validated Clinical Tool
First things first: you need to choose the right instrument. Your top priority should be a tool that's not only clinically validated but also built for the real-world pace of a busy clinic or care home.
A platform like Orange Neurosciences' OrangeCheck, for instance, is designed for this very purpose. It provides a quick yet thorough assessment that can be easily handled by a medical assistant or front-desk staff. This frees up the physician’s time while still gathering crucial data. When you're weighing your options, ask some practical questions:
Is it validated? Look for solid proof that the test holds up against established neuropsychological benchmarks.
Is it efficient? How long does it actually take? An assessment that’s around 15-20 minutes is usually manageable within a standard appointment slot.
Is the report clear? The output needs to be an easy-to-read report that gives you actionable information at a glance, not just a mess of raw numbers.
Step 2: Establish Clear Administration Protocols
Once you've picked your tool, you need to decide exactly how it will be used. Consistency is everything here. By creating a standard protocol, you eliminate guesswork and ensure screening is applied fairly to all your patients.
The best workflows embed cognitive screening right into existing appointments, making it feel like a natural part of the patient's visit. This helps normalize brain health check-ups and boosts participation.
Think about integrating the test at key touchpoints. For a primary care practice, the Annual Wellness Visit is the perfect opportunity. In a senior living community, it could be part of the intake process for a new resident or folded into an annual health review. A structured approach like this ensures nobody slips through the cracks.
Step 3: Train Your Team and Integrate the Data
Your team is the key to making this all work. Everyone, from the front desk to the nursing staff, needs to understand why you’re doing this and what their specific role is. The training should be practical and hands-on.
Practical Example: A Waiting Room Workflow
Patient Check-In: The receptionist lets the patient know they’ll be doing a "routine brain health check-up" on a tablet while they wait, framing it as a standard part of their visit.
Administration: A medical assistant hands the patient a sanitized tablet, gives them simple instructions, and makes sure they're comfortable getting started.
Data Integration: Once finished, the results are automatically and securely uploaded to the patient’s Electronic Health Record (EHR). By the time the doctor walks into the exam room, the report is already there to review alongside vitals.
Clinical Encounter: The physician can now use this objective data to guide the conversation, saving precious time and focusing the discussion on what matters.
For healthcare providers looking to put these systems in place, a model like this streamlines the entire process.
In California, demographic realities underscore just how important accessible online dementia tests are. State-level data shows that Black and Latino older adults are disproportionately affected by Alzheimer’s disease. These disparities are made worse by barriers like transportation challenges and a shortage of specialists, which makes web-based screening a genuinely practical tool for improving health equity. The need for brief, validated digital tools to flag concerns and guide referrals is becoming clearer every day.
Tying It All Together with Orange Neurosciences
As we've explored, online tests for dementia can be incredibly powerful screening tools. They're not here to replace a clinician's expert judgment, but to sharpen it. They provide the objective, data-driven insights needed to move conversations about brain health from subjective observation to standardized measurement—a critical step for proactive care.
But this is precisely where a dedicated clinical instrument becomes non-negotiable. The challenges of validity, seamless workflow integration, and clear, actionable reporting demand a solution built for the realities of modern practice. A consumer brain game or a generic questionnaire just won't cut it when you're making decisions that shape a patient's care journey.
The Orange Neurosciences Solution
This is exactly why we built our platform at Orange Neurosciences. Our assessments are designed to be both rapid and precise, measuring function across the key cognitive domains that matter—from memory and attention to executive function. The result is a comprehensive yet efficient cognitive profile, delivered in under 30 minutes, that fits neatly into your existing clinical workflow.
We designed OrangeCheck to be the practical link between an initial concern and confident clinical action. It delivers the clear, reliable data you need to guide your next step, whether that’s watchful waiting, further in-clinic investigation, or a specialist referral.
For clinicians and care facility managers, our system offers a straightforward path to elevating the standard of care.
Objective Data: Move beyond guesswork with validated, quantifiable cognitive metrics that paint a clear picture.
Workflow Efficiency: Have patients complete the assessment in the waiting room or during intake. You'll have valuable data before the appointment even starts.
Clear Reporting: Get reports that are easy to interpret, making it simple to spot and track cognitive changes over time.
By bringing a tool like OrangeCheck into your practice, you standardize your approach to cognitive screening. It ensures every single individual receives the same high level of proactive attention. We invite you to explore our solution and see for yourself how it can be implemented in your practice or facility.
Ready to see how objective cognitive data can transform your patient care? Schedule a demo with our team today and witness how OrangeCheck provides the clarity you need to make better-informed decisions about brain health.
Your Questions About Online Dementia Tests, Answered
We get a lot of questions from clinicians and caregivers about using online tests for dementia. Let's clear up some of the most common ones with quick, straightforward answers.
Can an Online Test Actually Diagnose Dementia?
No, and it's vital we're crystal clear on this. Online tests are screening tools, not diagnostic ones. Period. Their job is to flag potential cognitive changes that might warrant a closer look from a professional.
A formal dementia diagnosis is a serious medical conclusion. It can only be made by a qualified healthcare professional after a deep dive into the patient's health, which usually involves a full medical history, physical exams, lab work, and sometimes even brain imaging.
Here’s a good way to think about it: an online test is like a smoke detector. It can alert you to the possibility of a fire, but it can't tell you where the fire is, how big it is, or what caused it. The results are simply a piece of data, a signal that a full clinical workup might be the right next step.
How Do I Pick a Good Online Cognitive Test?
With so many options out there, choosing a reliable tool is key to feeling confident in the results. The most important thing to look for is whether a platform is "clinically validated." That's the industry's way of saying its performance has been rigorously tested against the gold-standard neuropsychological tests in proper scientific studies.
Beyond that, think about the practical side of things:
Is it easy to use? The interface needs to be simple enough for patients who aren't tech-savvy. Think large buttons, clear audio instructions, and a straightforward process.
Is the report useful? You need more than just a single, vague score. A good report breaks down performance across key cognitive areas like memory, attention, and executive function, giving you something truly actionable to discuss.
Is patient data safe? Make sure the platform is serious about privacy and complies with regulations like PHIPA or HIPAA. Patient confidentiality is non-negotiable.
What's the Next Step if a Patient's Score is Concerning?
First, don't panic. A concerning score is the start of a conversation, not the end of one. Your first move should be to sit down with the patient and their family to discuss the results calmly. It’s crucial to place that score within the larger context of their overall health, lifestyle, and any symptoms they've been experiencing.
A low score is just one piece of the puzzle. The most appropriate next step is a collaborative clinical investigation to understand the full picture.
From there, the investigation usually involves ruling out other common culprits for cognitive changes—things like vitamin deficiencies, thyroid issues, or medication side effects. After that, you might decide to conduct a more thorough in-office assessment yourself or refer the patient to a specialist, like a neurologist, for a full diagnostic evaluation.
At Orange Neurosciences, our entire mission is to give clinicians the precise, validated tools you need to make these crucial decisions with confidence. Our OrangeCheck assessment is designed to provide that objective cognitive data, helping you support early detection and guide patients toward the right care pathways.
Ready to see how reliable cognitive screening can fit into your practice? Book your personalised demo of OrangeCheck today.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


