Mini Cog Cognitive Assessment: Quick, Practical Guide
Jan 17, 2026

In a busy clinic, time is the one thing you can never get back. That's where the Mini-Cog cognitive assessment comes in—it’s a remarkably powerful screening tool that can flag potential cognitive impairment in just three to five minutes. It cleverly combines a simple three-word recall test with a clock-drawing task to give you a quick, yet insightful, snapshot of a patient's memory and executive function. This guide provides actionable insights and practical examples to help you master this essential tool.
What Is the Mini-Cog Cognitive Assessment?

The Mini-Cog was built for the realities of clinical practice. It was developed as a fast, reliable first step to spot patients who might need a more thorough workup for conditions like dementia or other forms of cognitive decline.
Think of it as a vital sign for brain health. You wouldn't skip a blood pressure check to screen for hypertension; in the same way, the Mini-Cog helps you catch cognitive red flags that might otherwise fly under the radar during a routine appointment. For example, if a patient mentions they've been misplacing keys more often, a quick Mini-Cog can help you determine if this is a normal part of aging or a signal that warrants a closer look.
The Two Core Components
The test's genius is in its simplicity and the different cognitive skills it probes. The whole assessment boils down to two key parts:
Three-Word Recall: This is a direct test of short-term memory. You ask the patient to remember three unrelated words (like "Leader, Season, Table") and then ask them to repeat the words back to you a few minutes later.
Clock-Drawing Test (CDT): This part might look simple, but it's a powerhouse. By asking a patient to draw a clock face with all the numbers and set the hands to a specific time, you're evaluating multiple abilities at once—planning, visual-spatial skills, and even abstract thinking.
This two-pronged approach makes the Mini-Cog a surprisingly robust screen. If a patient struggles to recall the words or can't draw the clock accurately, that’s a strong, early signal that more investigation is needed. You can learn more about where tools like this fit into the bigger picture in our guide on what is cognitive assessment.
It's important to remember that the Mini-Cog isn’t a diagnostic tool on its own. Its real job is to be a highly efficient red flag, helping you quickly identify at-risk individuals who should be referred for more detailed neuropsychological testing.
This kind of efficiency is becoming more critical every day. In 2023, the cognitive assessment segment commanded a 56.20% market share, a number that shows just how central these tools are becoming in early diagnosis and care planning for neurological conditions. This trend highlights the growing demand for reliable, rapid screeners just like the Mini-Cog.
How to Administer the Mini-Cog Step by Step
Running the Mini-Cog is a refreshingly simple process, which is exactly why it’s so widely used in busy clinical settings. Getting it right comes down to giving clear, consistent instructions and making sure the patient feels at ease. All you need is a pen and a blank piece of paper.
First, find a quiet space where you won't be interrupted. A patient's anxiety can easily skew the results, so a calm, reassuring tone goes a long way. Let them know you're just going to do a quick memory check that involves a few words and drawing a clock.
Step 1: Three-Word Registration
The first part of the test is all about immediate recall. The goal is to say three unrelated words and confirm the patient can hear and repeat them right back to you.
Pick three common nouns from different categories. Think along the lines of "Leader, Season, Table" or "Apple, Watch, Penny." Using different categories prevents them from being easily chunked together.
Speak clearly and at a steady pace. You can say something like, "I'm going to say three words for you to remember. After I say them, I want you to repeat them back to me."
State your three chosen words. For instance, "Leader, Season, Table."
Ask the patient to repeat them immediately. It's okay to repeat the words up to three times to make sure they've got them, but don't offer any other help or coaching.
This first step simply confirms the patient heard the words and can hold them in their mind for a few seconds. The real memory test comes a bit later.
Step 2: The Clock-Drawing Task
As soon as they've repeated the words, you'll move on to the clock drawing. This isn't just about drawing; it taps into visuospatial skills, planning, and executive function.
The clock-drawing test is a powerful little tool on its own. If you're curious about the deeper mechanics, we've covered the essentials of dementia screening clock tests in another guide.
For the Mini-Cog, hand the patient the blank paper and pen. Your instruction should be given all at once, not broken into pieces.
"Next, I'd like you to draw a clock for me. First, draw a large circle. Then, put in all the numbers where they belong on the clock face. Finally, set the hands to show the time ten past eleven."
Giving the entire instruction at once is crucial. It tests their ability to understand and execute a multi-step command. As they draw, pay attention to their process—how they plan the spacing of the numbers, any hesitations, or corrections. These observations can offer rich clinical insights beyond the final score.
Step 3: Three-Word Recall
After the clock is complete, it's time for the final step: testing delayed recall. This is the moment you find out if those three words from the beginning made it into short-term memory.
Simply ask the patient, "What were the three words I asked you to remember earlier?"
It's important not to give any clues or prompts. Just record how many words they recall correctly on their own. And that's it—you've finished the test and have everything you need for scoring.
To help clinicians, here is a quick-reference table summarizing the protocol.
Mini-Cog Administration and Scoring Protocol
Step | Instruction to Patient | Scoring Criteria |
|---|---|---|
1. Word Registration | "Listen carefully. I am going to say three words that I want you to repeat back to me now and try to remember. The words are [word 1, word 2, word 3]." | No score is assigned for this step. The purpose is to ensure the patient can hear and repeat the words. |
2. Clock Drawing | "Next, I want you to draw a clock. Put in all the numbers and set the time to ten past eleven." | Normal Clock (2 points): All numbers are present in the correct sequence and approximate position, and the hands correctly display the specified time. |
Abnormal Clock (0 points): Any errors in number placement, sequence, or hand position. | ||
3. Word Recall | "What were the three words I asked you to remember?" | 1 point is awarded for each word recalled correctly without any cues. (Total possible score: 3 points) |
This table provides a concise summary, but the real art is in the smooth, confident delivery of the instructions.
Struggling to keep track of screenings and results? The Orange Neurosciences platform offers digital tools that standardize administration and automate scoring, taking the guesswork out of the process. Visit our website or email our team today to learn how our AI-powered solutions can fit into your clinical workflow.
Scoring and Interpreting Mini Cog Results
Once you've administered the Mini-Cog, the next step is scoring. Thankfully, this part is refreshingly simple and objective. The entire assessment is scored on a five-point scale, combining the results from the word recall and the clock-drawing task to give you a clear, actionable number.
This simplicity is by design, making it perfect for a busy clinical setting. You won't need to consult complex scoring manuals to figure out what the results mean. Let's break down exactly how to turn the patient's responses into a meaningful score.
The Simple Five-Point Scoring System
The scoring system is straightforward and broken into two parts. You just need to assign points based on how the patient performed on each component.
Word Recall (0–3 points): The patient gets one point for each of the three words they remember correctly without any hints.
Clock-Drawing Test (0 or 2 points): This part is all or nothing—it's either normal or it's not. A patient receives two points for a normal clock and zero points for an abnormal one.
So, what counts as a "normal" clock? It needs to have all the numbers in the right sequence and in roughly the correct positions. Crucially, the hands must also show the correct time you asked for (like ten past eleven). Any major errors—missing numbers, incorrect placement, or the wrong hand positions—mean a score of zero for this section.
Translating the Score into Clinical Action
The final score, ranging from 0 to 5, gives you a solid indicator of the likelihood of cognitive impairment. This isn't a final diagnosis, of course, but it’s a powerful screening result that tells you whether a more comprehensive workup is needed.
Here’s how to interpret the final tally from the Mini-Cog:
Score of 0–2 (Positive Screen): A patient scoring in this range is highly likely to have cognitive impairment. Actionable Insight: This score should trigger an immediate referral for a full diagnostic evaluation, including more comprehensive neuropsychological testing and a review of their medical history.
Score of 3–5 (Negative Screen): This result suggests significant cognitive impairment is unlikely. Actionable Insight: While reassuring, this doesn't rule out very mild impairment. Your next step should be to document the score and plan for a routine follow-up, perhaps annually, unless new concerns arise.
This flowchart gives you a great visual guide for the whole process, from administration to the final score.
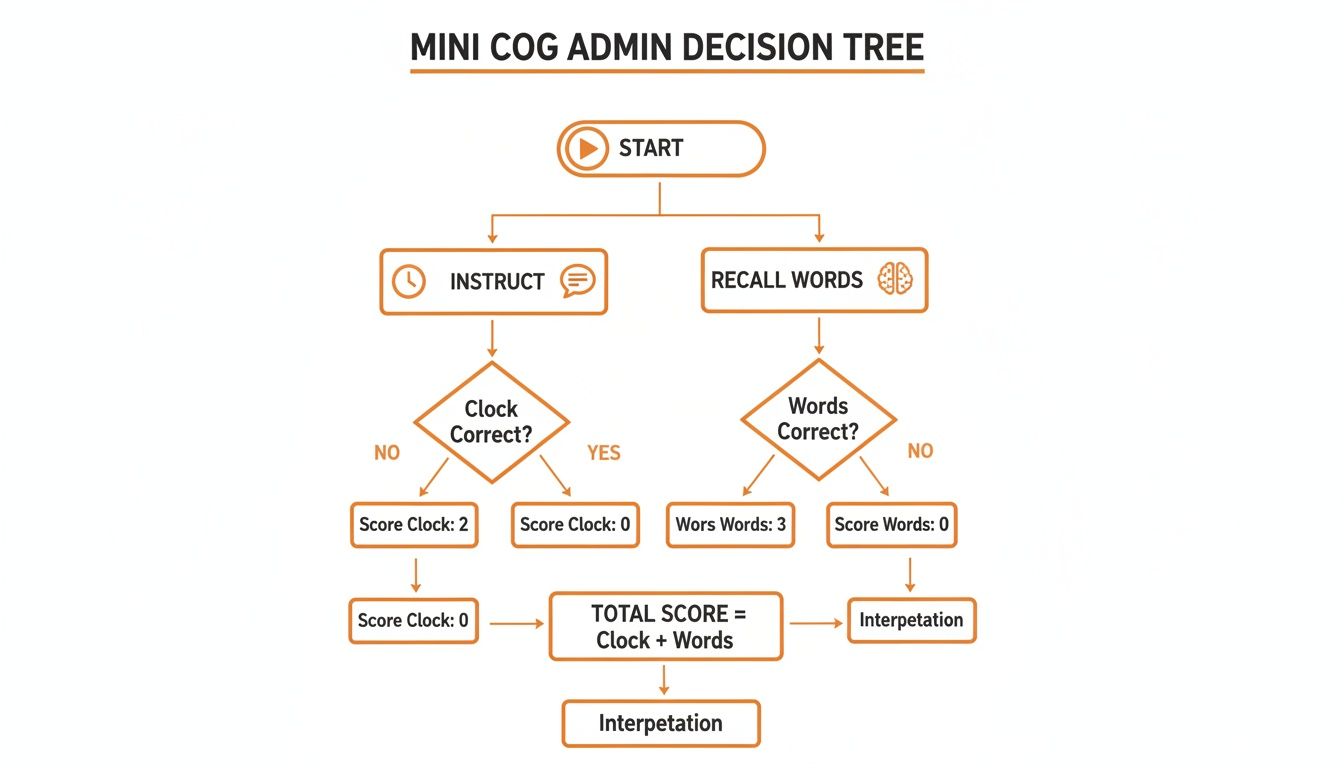
This visual decision tree really helps standardize the assessment, making sure every clinician follows the same path from initial instruction to the final, interpretable result.
It's important to remember that context matters. A score of 3, for instance, might warrant closer observation or a follow-up screening in six months, especially if there are other clinical concerns. The Mini-Cog score is one piece of a larger clinical puzzle.
While the Mini-Cog is an excellent first-line tool, some situations may require a more detailed assessment right from the start. For a deeper look at how scoring works in other common screeners, you can check out our guide on MMSE scoring and interpretation, which offers a great comparative perspective.
Ultimately, mastering the Mini-Cog's scoring empowers you to make confident, evidence-based decisions, ensuring that at-risk patients get the timely follow-up they need.
Understanding the Clinical Value of the Mini Cog
The Mini-Cog truly shines in fast-paced clinical settings where time is a precious commodity. Picture a busy primary care office, a bustling hospital ward, or even a routine wellness check in a long-term care home. In these places, its practical value is clear—it acts as a quick, effective first line of defence for flagging potential cognitive issues.
The power of this mini cog cognitive assessment is rooted in its solid diagnostic accuracy. Its sensitivity, which is the ability to correctly identify people who have cognitive impairment, is consistently high for dementia. At the same time, its specificity is strong enough to correctly identify those who are cognitively healthy, which helps cut down on unnecessary follow-up tests and the anxiety they can cause for patients.
Where the Mini Cog Excels
This tool is especially useful in certain populations and settings because its design minimizes biases that can pop up due to education level or language barriers.
Primary Care Settings: It gives a family doctor a quick, evidence-based reason to dig deeper into cognitive complaints during a standard appointment.
Hospitals: The Mini-Cog can be used right at the bedside to screen for things like delirium or an underlying dementia that could complicate a patient's care plan.
Diverse Populations: Because it doesn’t rely on complex language skills like many other screeners, it performs well across a wide range of cultural and educational backgrounds.
The Mini-Cog's real strength is its ability to send a clear signal through the noise of a busy clinic. A low score is a powerful indicator that prompts a clinician to pause and say, "Okay, we need to look deeper into this."
This kind of efficiency is becoming more and more critical as the demand for reliable cognitive tools grows. The global cognitive assessment market is expected to hit USD 20.01 billion by 2030, a jump driven largely by the need for more streamlined testing methods. Clinical trials are currently the biggest players in this market, making up 34.2% of all applications as researchers look for objective data they can gather frequently. If you're interested in these trends, you can explore the full cognitive assessment industry report on mordorintelligence.com.
Knowing Its Limitations and Boundaries
Of course, no tool is perfect. Understanding the Mini-Cog’s limitations is the key to using it responsibly.
While it's excellent for spotting moderate to severe dementia, it’s not as good at catching mild cognitive impairment (MCI). A person in the very early stages of memory loss might still score in the normal range, which can create a false sense of security. If you're trying to tell the difference between these conditions, our guide on mild cognitive impairment vs. dementia can offer more clarity.
A few other factors can also muddy the waters and require some clinical judgment:
Severe hearing or vision loss can obviously make it hard for a patient to hear the instructions or see well enough to draw the clock.
Significant motor impairments, like severe arthritis or tremors from Parkinson's disease, can make the clock-drawing part a real challenge.
Low educational attainment or illiteracy can have an impact, though less so than with tests that are heavy on language.
Keeping these boundaries in mind helps you interpret the results with the right context. It helps you decide when a more comprehensive assessment is the right call. If you have a gut feeling that MCI might be at play or if other health issues could be affecting the score, reaching for a more detailed tool is always the best next step.
Taking the Mini-Cog Digital
The classic pen-and-paper Mini-Cog is a fantastic tool, no doubt. But stepping up to a digital cognitive assessment platform is like trading in a trusty paper map for a live GPS. Both will get you where you're going, but one offers real-time data, tracks your progress effortlessly, and takes the guesswork out of the equation.
Digital versions of the mini cog cognitive assessment and other screeners deliver immediate, practical benefits right out of the box. They automate the scoring, which gets rid of the risk of human error and the little subjective judgments that can creep in, especially when scoring a clock drawing. This creates a consistent standard, ensuring every single assessment is scored the same way, regardless of who's administering it.
This screenshot from the Orange Neurosciences platform gives you a sense of how a well-designed digital interface can turn complex cognitive data into something intuitive and easy to grasp.

This kind of clear, visual reporting helps clinicians see a patient's cognitive profile at a glance and track subtle shifts over time with much greater precision than ever before.
What AI-Powered Platforms Bring to the Table
Today's digital platforms are much more than just simple automation. They use AI to uncover deeper insights that a basic screening score just can't provide.
Instead of a single number, these systems can generate a detailed cognitive profile that breaks down performance across different domains like memory, attention, and executive function. This more nuanced data is exactly what you need to build more precise and effective care plans for your patients.
The impact on a clinical workflow is huge:
Secure Data Storage: Every result is stored securely, building a longitudinal record that makes it simple to monitor a patient’s cognitive health over months or years.
EHR Integration: Many platforms plug directly into Electronic Health Record (EHR) systems. This puts cognitive data right alongside other vital health information, giving you a truly holistic view of the patient.
Objective Analysis: AI-driven tools can spot subtle patterns in responses—things like hesitation times or specific drawing patterns—that are invisible to the human eye. This adds another powerful layer of objective data to your assessment.
The Clear Trend Toward Digital Cognitive Tools
The healthcare world is steadily moving in this direction. Software-based solutions are now the dominant force, capturing 72.7% of the market share in 2024. This isn't just a fad; it reflects a clear clinical preference for the scalability and data-driven insights that digital platforms offer.
While pen-and-paper tests still have their place, the momentum is undeniably with digital. This is driven by ongoing advancements in AI and machine learning that are making these tools more accurate and valuable all the time.
This shift allows clinicians to move beyond a simple pass/fail screening. It opens the door to a more proactive, data-informed approach to brain health, helping us identify at-risk individuals earlier and with far more confidence.
Of course, once a digital assessment tool is in place, the work doesn't stop. Continuous improvement relies on measuring its impact and user engagement. For those curious about the technical side of optimizing these tools, understanding the best analytics tools for mobile apps can offer some valuable lessons.
Ultimately, integrating these modern platforms transforms the mini cog cognitive assessment from a standalone screener into a key part of a dynamic, ongoing cognitive care strategy. To get a better idea of how these tools could work in your practice, check out our guide on cognitive assessment online.
Common Questions About the Mini Cog Assessment
Even with a tool as straightforward as the Mini-Cog, questions always pop up in the real world of clinical practice. Getting a handle on these common scenarios and nuances is key to feeling confident and making sure you’re getting the most out of the assessment. Let's walk through some of the most frequent questions clinicians have about this powerful little screener.
Think of this as your troubleshooting guide to help you integrate the mini cog cognitive assessment smoothly into your patient care workflow.
Can It Be Used with Patients from Diverse Backgrounds?
Absolutely. One of the greatest strengths of the Mini-Cog is its design; it’s far less dependent on a patient's primary language or formal education than many other screeners. This makes it a fantastic tool for working with diverse populations.
For the three-word recall, you can simply choose words the patient will have no trouble understanding. If you're working with a translator, their job is just to provide a direct, literal translation—no hints or extra context allowed.
The clock-drawing portion is largely a non-verbal test of executive function and visuospatial skills, which holds up well across different cultures. That said, always be mindful of physical limitations. Severe arthritis or significant visual impairment could make drawing difficult, so be sure to note those factors in the patient’s file.
What Should I Do with an Intermediate Score?
A score that lands in the middle, like a 3 out of 5, isn't a clear pass or fail. Instead, think of it as a yellow light—a signal that you need to slow down and investigate further to see the full picture.
An intermediate score isn't a final answer. It's a critical data point that tells you it's time to gather more context.
Your best next move is to start digging deeper. This could mean:
Taking a detailed cognitive history: Chat with both the patient and a family member or caregiver. Ask about any changes they’ve noticed in memory, problem-solving, or how they're handling daily tasks.
Assessing functional abilities: Ask practical questions. Are they managing their medications correctly? Are they having any trouble with finances or getting around familiar places?
Considering a more detailed tool: An ambiguous Mini-Cog result is the perfect reason to bring in a more comprehensive assessment. The Montreal Cognitive Assessment (MoCA), for example, is much better at picking up on milder forms of cognitive impairment.
How Often Should I Repeat the Mini Cog?
There's no rigid, one-size-fits-all schedule here. The right frequency for re-testing depends entirely on the clinical situation. The goal is to use the mini cog cognitive assessment to track meaningful changes over time.
For a patient with a normal baseline score and no new cognitive complaints, an annual screening is usually plenty. But for someone with an intermediate score or other clinical red flags, you’ll want to track their cognitive path more closely, maybe re-testing every six to twelve months.
It’s also smart practice to repeat the test after a major health event like a stroke, a serious infection, or a hospital stay. This helps you establish a new cognitive baseline. Ultimately, it’s the consistent documentation of these scores over time that will allow you to spot concerning trends early on.
At Orange Neurosciences, we believe that better data leads to better care decisions. Our AI-powered digital platform provides objective, detailed cognitive profiles that go far beyond a simple screening score, helping you create more precise and effective patient care plans. Discover how our tools can bring clarity to your clinical workflow by visiting https://orangeneurosciences.ca today.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


