A Clinician's Guide to the Mini Cog Assessment
Feb 14, 2026

When you only have a few moments with a patient, you need a screening tool that is fast, reliable, and straightforward. That's exactly where the Mini-Cog comes in. In just three minutes, this simple test can help detect cognitive impairment by giving you a quick snapshot of a person's memory and executive function.
Your Quick Guide to the Mini Cog Assessment
In a bustling primary care office, time is always a luxury. You need a way to quickly and efficiently flag patients who might be experiencing cognitive changes, without pulling out a lengthy, complicated evaluation for every person. The mini cog assessment is the perfect fit for this challenge, serving as an effective first-line screener.
Think of it like a "check engine" light for the brain. It won't give you a full diagnostic report, but it’s a remarkably reliable signal that a deeper look is warranted. This is absolutely critical for catching conditions like dementia or other forms of cognitive decline as early as possible. If you're looking to understand the bigger picture, you can explore our detailed guide on what is a cognitive assessment.
The Two Core Components
The true power of the Mini-Cog lies in its elegant simplicity. It combines two distinct tasks that probe different, yet related, cognitive areas:
Three-Word Recall: This is a direct test of short-term memory. You ask the patient to remember three unrelated words—like "banana, sunrise, chair"—and then ask them to repeat them back to you a few minutes later.
Clock-Drawing Test (CDT): This single task assesses multiple cognitive abilities at once, including planning, visuospatial skills, and abstract thinking. The individual has to draw a clock face, put all the numbers in the correct spots, and then draw the hands to show a specific time.
For instance, successfully drawing a clock to show "10 minutes past 11" isn't as simple as it sounds. It requires understanding the command, planning the circular layout of 12 numbers, and then translating an abstract concept of time into a concrete visual. A small error in any of these steps could signal an underlying issue.
Combining these two tasks is what makes the Mini-Cog so effective. It’s not just about memory; it's about seeing how different parts of the brain work together.
For a tool this brief, its accuracy is impressive. The Mini-Cog has a sensitivity of 76% and a specificity of 89% for detecting cognitive impairment in a primary care setting, making it one of the most trusted screeners available. This blend of efficiency and reliability makes it an indispensable tool for any healthcare professional focused on proactive cognitive care.
Here’s a quick summary to keep on hand.
Mini Cog Assessment at a Glance
This table breaks down the essential features of the Mini-Cog, giving clinicians a quick reference for understanding its components and purpose.
Feature | Description |
|---|---|
Administration Time | Approximately 3 minutes. |
Core Components | Three-Word Recall (tests short-term memory) and the Clock-Drawing Test (tests executive function, planning, and visuospatial skills). |
Target Population | Primarily older adults in various settings, including primary care, hospitals, and community health centres. |
Primary Purpose | A rapid screening tool to detect potential cognitive impairment and determine if further, more comprehensive evaluation is needed. |
Scoring System | A simple 5-point scale based on the number of words recalled (0-3 points) and whether the clock is drawn correctly (0 or 2 points). Scores of 0-2 suggest positive for impairment. |
Key Strengths | Quick to administer, easy to score, minimal training required, and less affected by language or educational background compared to other screeners. |
This streamlined approach allows for widespread screening, ensuring more individuals who need follow-up care are identified early on.
How to Administer the Mini-Cog in 3 Steps
Running the Mini-Cog is a refreshingly simple process, built for speed and clarity right in the middle of a busy clinic day. The key to getting good results is creating a calm, supportive space where the person feels comfortable and not rushed. The whole test boils down to three straightforward steps.
Following this protocol every time is crucial. It means the results you get today are reliable and can be accurately compared to results you might get six months from now. This isn't about guesswork; it's about a standardized approach that any healthcare provider can use consistently.
Step 1: Repeat and Remember the Words
The first step jumps right into testing immediate recall and memory registration. Your job is to say three common, unrelated words and make sure the individual has actually heard and can repeat them back to you.
Start by saying, "I am going to say three words that I want you to repeat back to me now and try to remember. The words are banana, sunrise, chair."
Listen closely as they repeat the words. If they miss one or two on the first go, you can say them again, up to two more times. The goal here is just to ensure the information has been successfully logged in their brain. The real memory test comes later.
Step 2: Complete the Clock Drawing Test
Next, you'll get a snapshot of their visuospatial skills, planning, and executive function with the clock-drawing test. This isn't just a drawing exercise; it’s a window into how the brain organizes and carries out a multi-part command.
Hand the person a blank piece of paper and a pen. Give them these instructions clearly, all at once, without breaking them down:
"Please draw a large circle for me to represent a clock face."
"Now, put all the numbers where they should go on a clock."
"And finally, set the hands to show 10 minutes past 11."
Resist the urge to help or correct them as they draw. The way they tackle the task—how they place the numbers, the spacing, the final position of the hands—provides a ton of clinical insight. It's a simple request that relies on complex cognitive coordination. If you're interested in other screening tools, our guide on the Montreal Cognitive Assessment instructions provides more examples.
Step 3: Recall the Three Words
The final step brings us full circle, back to memory. After the clock-drawing task has acted as a short distraction, you'll ask the person to pull up those three words from the beginning.
Simply ask, "What were the three words I asked you to remember earlier?"
Practical Example: A patient recalls "banana" and "chair" but forgets "sunrise." They would score 2 out of 3 on this portion. Another patient might not remember any words at all, scoring a 0. This simple recall task is surprisingly powerful for flagging potential memory issues that need a closer look.
By following these three steps, you can confidently run the Mini-Cog. This quick screen gives you a valuable first look into a person's cognitive health, helping you decide if a more detailed evaluation is the right next step.
Scoring and Interpreting Mini Cog Results
Once you've administered the Mini-Cog, the next step is to translate your patient's performance into a clear, actionable score. Thankfully, this process is refreshingly straightforward and designed for quick interpretation in a busy clinical setting. The scoring system combines the results from both the word recall and the clock-drawing tasks into a simple 5-point scale.
The final score is calculated by adding the points from each component:
Word Recall: The patient gets one point for each of the three words they correctly remember without any prompting. This gives a possible score of 0 to 3.
Clock-Drawing Test: This task is scored on a simple pass/fail basis. A correctly drawn clock—with all the numbers and the hands pointing to the right time—receives 2 points. Any significant error means a score of 0 points.
This method gives you a quick, quantitative measure of cognitive function. Properly interpreting these results often means having a good grasp of the definition of normative data to see how an individual’s score stacks up against established benchmarks for their age and background.
From Score to Screening Outcome
So, you have a final score between 0 and 5. Now what? A simple algorithm helps you decide whether the result is negative (meaning the person is likely cognitively intact) or positive (suggesting possible cognitive impairment), which signals the need for a closer look.
This table breaks down how to combine the word recall and clock draw results to arrive at a final screening outcome.
Mini Cog Scoring Algorithm | ||
|---|---|---|
Word Recall Score | Clock Draw Result | Interpretation (Screening Result) |
0, 1, or 2 | Abnormal | Positive Screen (Possible Dementia) |
0, 1, or 2 | Normal | Positive Screen (Possible Dementia) |
3 | Abnormal | Positive Screen (Possible Dementia) |
3 | Normal | Negative Screen (Cognitively Intact) |
Essentially, the process is streamlined to give you a clear direction, removing ambiguity from the initial screening.
Making Sense of the Final Score
The combined score, from 0 to 5, determines the screening outcome. The interpretation is refreshingly direct:
A total score of 0, 1, or 2 is considered a positive screen. This result suggests a high likelihood of cognitive impairment, and a more comprehensive diagnostic workup is strongly recommended.
A total score of 3, 4, or 5 is considered a negative screen. This indicates that cognitive impairment is unlikely.
Actionable Insight: A patient recalls only one word (1 point) and draws an incorrect clock (0 points). Their total score is 1. This is a clear positive screen. Your next action should be scheduling a follow-up for a more detailed assessment and discussing the results with the patient or their family.
This flowchart gives you a great visual guide for the decision-making process.
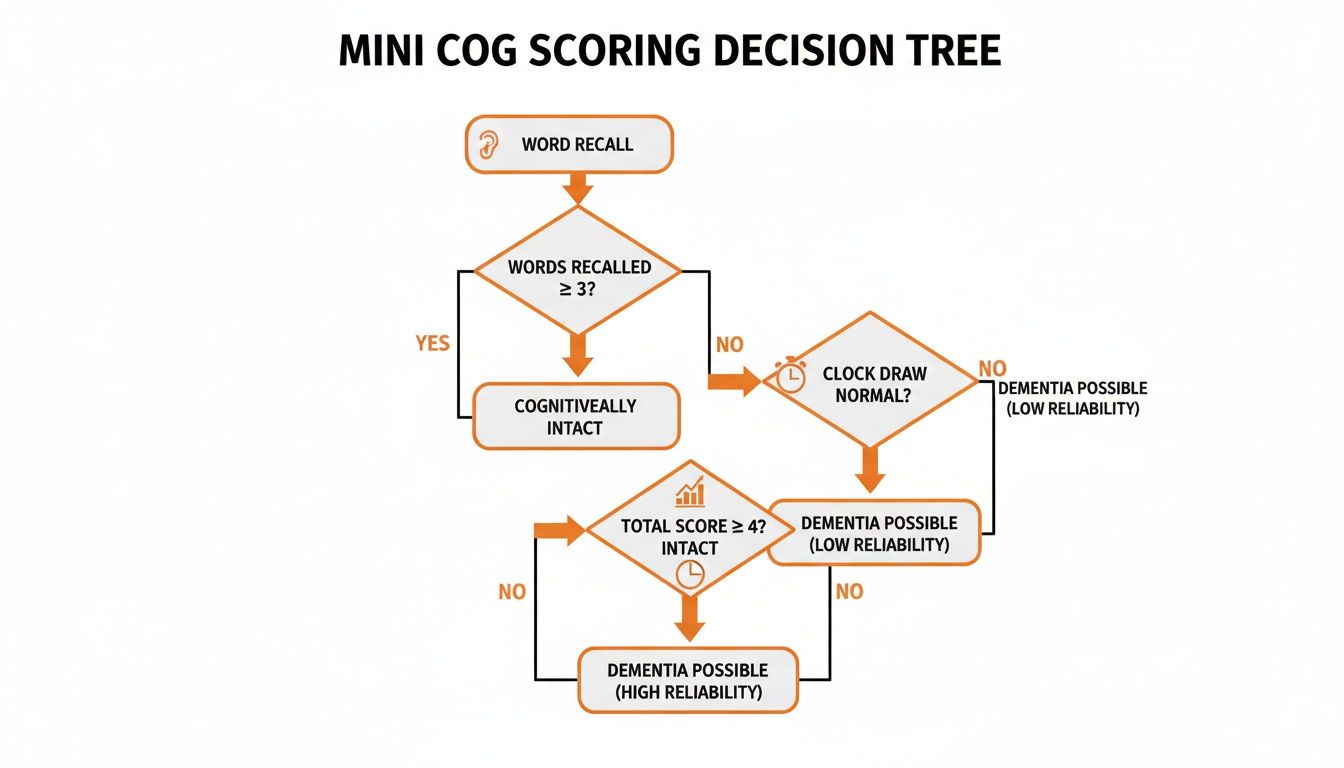
As you can see, the decision tree clearly shows how the word recall and clock draw results come together to produce a final interpretation, making it easy to integrate into any clinical workflow.
From Score to Actionable Insight
Interpreting the Mini-Cog isn't just about the number; it’s about what you do with that information. A patient scoring a 2 is a clear signal to investigate further. But what about a score of 3 or 4? While technically negative, it might still warrant a conversation, especially if you have other clinical concerns.
You can learn more about how different cognitive screening scores work by reading our guide on MMSE scoring and interpretation.
This clear-cut system removes the guesswork. It empowers clinicians to confidently identify individuals who need a deeper cognitive evaluation. By transforming a three-minute interaction into a vital data point, the Mini-Cog helps you take decisive next steps in patient care.
And when you do need to move beyond screening, that's where platforms like Orange Neurosciences can step in, providing the in-depth cognitive profiling needed to build a complete picture of a patient’s brain health. For more information, we invite you to visit our website or send us an email to see how our platform can integrate with your practice.
When to Use the Mini Cog Assessment
Knowing the right time and place to use the Mini-Cog is key to unlocking its power as a rapid screening tool. Its real strength is in its simplicity and speed, making it a perfect fit for settings where time is tight, but the need for a quick cognitive snapshot is high. The Mini-Cog shines when used proactively to flag potential issues early, long before they become more obvious problems.
Think of it as a vital sign for brain health. In the same way you’d routinely check blood pressure, the Mini-Cog can be seamlessly woven into regular appointments to get a baseline and track any cognitive changes down the road.
Ideal Clinical Applications
The Mini-Cog isn't a silver bullet for every situation, but in certain scenarios, its efficiency is second to none. It’s most valuable in fast-paced environments where a long, drawn-out assessment just isn't practical for a first look.
Here are a few real-world examples where the Mini-Cog is a great fit:
Routine Senior Wellness Exams: For older adults, especially those over 65, the Mini-Cog is a fantastic annual check-up tool to catch subtle cognitive shifts that might otherwise be missed.
Busy Primary Care Offices: When a patient or family member brings up concerns about memory lapses or confusion, the Mini-Cog gives you a quick, evidence-based starting point in under five minutes.
Preoperative Cognitive Checks: Before a major surgery, getting a read on a patient's cognitive baseline can help clinicians anticipate risks for issues like postoperative delirium.
Its power lies in its knack for quickly and reliably spotting individuals who need a more thorough evaluation. This isn't just theory; recent research has backed its effectiveness across diverse groups of people. For instance, studies from Cedars-Sinai found it had an 82% accuracy in identifying mild cognitive impairment among 1,200 patients. That's a huge deal, especially when you consider that 1 in 9 Californians over 65 is living with Alzheimer's. You can discover more insights about the growing need for effective neurocognitive tools here.
Understanding Its Limitations
While it’s a powerful little tool, it’s critical to remember that the Mini-Cog is a screener, not a diagnostic tool. A positive result doesn't mean someone has dementia or any specific condition. It simply signals that a more comprehensive workup is needed.
Actionable Insight: If a patient has a positive screen, avoid using diagnostic terms like "dementia." Instead, explain the result clearly: "This quick screen suggests we should take a closer look at your memory and thinking skills. The next step is a more detailed evaluation to understand this better."
It’s also important to know when the Mini-Cog might be less effective or even produce misleading results. Its performance can be influenced by a few factors.
Keep these key limitations in mind:
Very Mild Cognitive Impairment: The test might not be sensitive enough to pick up on the earliest, most subtle signs of cognitive change.
Confounding Conditions: Things like severe depression, delirium, uncorrected vision or hearing loss, or major motor impairments that make clock drawing difficult can skew the results.
Educational and Cultural Bias: While it’s less biased than many other screeners, a person’s background can still play a role in their performance, especially with the clock-drawing task.
By understanding both its strengths and its limitations, you can use the mini cog assessment responsibly in your practice. It's an invaluable first step in the cognitive care journey, helping you make informed decisions about who needs a deeper, more detailed look. And when that deeper dive is needed, platforms like Orange Neurosciences can provide that next level of objective cognitive profiling.
Comparing the Mini-Cog to Other Screening Tools
Choosing the right cognitive screener often feels like a balancing act between thoroughness and time. In a busy clinic, every single minute counts, which makes the Mini-Cog assessment an incredibly attractive option. But how does its rapid, three-minute format really stack up against more detailed tools like the Mini-Mental State Examination (MMSE) or the Montreal Cognitive Assessment (MoCA)?
The biggest selling point of the Mini-Cog is its sheer efficiency. While the MMSE can take 10-15 minutes and the MoCA hovers around 10 minutes, the Mini-Cog gives you a reliable snapshot in a fraction of that time. That speed is a game-changer for routine screenings during annual wellness visits or in high-volume primary care settings.
Key Differences at a Glance
The most important distinction comes down to complexity and focus. The MMSE and MoCA are much more comprehensive, casting a wider net over cognitive domains like orientation, language, and calculation. The Mini-Cog, on the other hand, zeroes in on two high-yield areas: short-term memory and executive function (via the clock-drawing test).
This focused approach also makes the Mini-Cog less prone to certain biases.
Practical Example: A patient who recently immigrated and is still learning English might struggle with the MMSE's language-heavy sections, leading to a score that doesn't accurately reflect their cognitive health. The Mini-Cog, with its simpler word recall and non-verbal clock test, offers a much fairer assessment in this scenario.
This isn't just theory; compelling evidence backs it up. A 2022 multicenter trial across 15 CA facilities found it detected 91% of dementia cases in under-served communities, outperforming the MMSE by a whopping 18% in sensitivity for non-English speakers. You can explore more data on the value of accessible cognitive tools in the latest market research.
For a deeper dive into these other tools, check out our detailed guide comparing the MoCA vs the MMSE.
Choosing the Right Tool for the Job
So, when should you reach for each tool? Think of the Mini-Cog as your go-to initial screener—a quick, effective way to flag potential concerns that need a closer look. If a patient scores poorly on the Mini-Cog, or if your clinical intuition is telling you something is off, progressing to a more detailed tool like the MoCA is a logical next step.
Here’s a practical way to think about it:
Screening Tool | Best For |
|---|---|
Mini-Cog | Rapid, routine screening in primary care; initial checks for memory concerns; testing diverse populations with varying language or education levels. |
MoCA | Evaluating patients with suspected mild cognitive impairment (MCI); assessing executive function in more detail; follow-up after a positive Mini-Cog screen. |
MMSE | Tracking the progression of moderate-to-severe dementia; situations where a widely recognized, older standard is required. |
Ultimately, the Mini-Cog excels in its designated role: a fast, fair, and reliable first-pass filter. It empowers clinicians to efficiently identify patients who need a more comprehensive evaluation, making sure valuable time is directed where it’s needed most.
Taking the Next Step After a Positive Screen
A positive result on the Mini-Cog is a critical signal, but it’s the beginning of a journey, not the final destination. Think of it like a smoke alarm; it’s incredibly effective at alerting you to a potential problem, but it doesn’t tell you the fire's location or its size. The immediate next step is to move from that general alert to a detailed investigation.
This is where a more granular analysis becomes essential. A positive screen raises important questions that the Mini-Cog was never designed to answer. Is the issue primarily memory-based, or are other cognitive domains like attention, processing speed, or executive function involved? Answering this requires a deeper, more objective look at the brain's overall performance.

From Screening to a Detailed Cognitive Profile
Transitioning from a simple screen to a comprehensive profile is crucial for creating an effective care plan. Platforms like Orange Neurosciences are built to provide this next level of insight, quickly and objectively. In under 30 minutes, our system moves beyond a basic screener to deliver a detailed, multi-domain cognitive profile.
This allows you to "zoom in" on the specific areas of concern flagged by the initial Mini-Cog. Our game-based modules, for example, can help pinpoint whether a patient's difficulty stems from slower processing speed or a deficit in sustained attention—a distinction that informs truly personalized intervention strategies. If a potential dementia diagnosis is a concern, families may also need to understand complex legal processes, such as how to get guardianship of a parent with dementia.
Actionable Insight: By assessing domains the Mini-Cog doesn't cover, you can build a complete picture of an individual's cognitive health. This objective data removes guesswork, helping you develop targeted care plans based on specific strengths and weaknesses.
To learn more about this crucial follow-up process, you might be interested in our guide on what is a neuropsychological assessment.
Discover how Orange Neurosciences can help you move seamlessly from initial screening to precise, data-driven intervention. Visit our website to see how our insights can enhance your care workflow.
Your Questions, Answered
When you're adding a new tool to your clinical practice, questions are a good thing. They show you're thinking critically about how and when to use it. Let's tackle some of the most common queries about the Mini-Cog so you can feel confident putting it to work.
How Accurate Is the Mini-Cog, Really?
For a test that takes just three minutes, the Mini-Cog packs a surprising punch. Research from primary care settings shows it has a sensitivity of 76% and a specificity of 89% for spotting cognitive impairment.
What does that mean in the real world? It means the test is quite good at flagging individuals who likely have cognitive issues (sensitivity) while also correctly giving the all-clear to those who don't (specificity).
Practical Example: If a patient only recalls one of the three words but manages to draw a perfect clock, their score of 3 is technically a negative screen. However, the poor recall is a valuable clinical clue. This allows you to say, "Your overall score is fine, but I've noted a small issue with memory. Let's make sure to check this again at your next visit." It gives you a quick, evidence-based data point that can catch subtle issues a simple conversation might miss.
Does a Person's Education Level Skew the Results?
This is one of the Mini-Cog's biggest advantages. Unlike many other cognitive screeners, it's far less influenced by a person's level of education or their primary language.
The tasks are simple and nearly universal: remember three everyday words and draw the face of a clock. These don't rely heavily on formal schooling. This design makes it a more equitable tool across diverse patient populations.
Of course, no test is perfect. In very rare cases, severe illiteracy or a complete lack of familiarity with analog clocks could affect the clock-drawing task. If you run into that situation, simply use your clinical judgment. You might weigh the word recall score more heavily or switch to an alternative screening tool.
What if a Patient Doesn't Want to Take the Test?
It happens. If a patient seems hesitant or anxious, the best approach is a supportive and gentle explanation. Frame it as a routine part of their check-up.
You could say something like, "This is just a quick check of your memory, much like how we check your blood pressure every time you're here." Keeping it low-key and emphasizing that it's a standard part of their overall health assessment can often put them at ease.
If they still refuse, it's crucial to respect their decision. Simply document the refusal and your reasons for wanting to perform the screen in their chart. From there, you can rely on your own clinical observations and information gathered from family members (with the patient's permission) to complete your assessment.
A quick screen is a powerful first step, but it's just that—a start. To see how you can move from a simple flag to a detailed cognitive profile with targeted interventions, explore what Orange Neurosciences can do. Our platform provides the deep, objective insights needed to create truly personalized care plans. Discover more at https://orangeneurosciences.ca.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


