A Clinician's Guide to Mental Health Screening Tools
Feb 28, 2026

Mental health screening tools are structured questionnaires or checklists that give clinicians a quick, objective way to spot individuals who might be at risk for a mental health condition. They aren't diagnostic tests. Instead, think of them as a crucial first step—much like taking a patient's blood pressure to flag potential issues that require a closer look. The actionable insight here is simple: use these tools to systematically identify risk early, not just when a patient is in crisis.
Why Mental Health Screening Is Now Essential
In modern healthcare, proactive mental health screening is no longer a "nice-to-have"—it's as vital as a routine physical health check. The days of relying solely on subjective observation are over. The need for objective, scalable assessment is clear. This shift helps clinicians solve a core challenge: how to efficiently and reliably identify patients in distress before their symptoms escalate.

This is where standardized mental health screening tools provide a structured framework, enabling you to take immediate, informed action.
The Smoke Detector for Mental Wellbeing
It helps to think of these tools as a "smoke detector" for mental wellbeing. Their purpose is to catch the earliest signs of distress—like emerging anxiety or depression—long before a situation escalates into a full-blown crisis. This early detection is the cornerstone of effective, actionable care.
For a practical example, a primary care physician can use the PHQ-9 (Patient Health Questionnaire-9) during an adult's annual check-up. If the patient’s score indicates moderate depressive symptoms, it provides an immediate, data-backed reason to start a conversation and create a follow-up plan. That simple, five-minute questionnaire becomes the catalyst for life-changing support.
By integrating objective screening, you can shift from a reactive to a proactive care model. The actionable insight is to systematically identify risk, not just wait for a patient to be in obvious crisis. This paves the way for timely support and dramatically improved outcomes.
Elevating the Standard of Care
Weaving formal screening processes into your practice normalizes conversations about mental health, chipping away at the stigma that often stops people from asking for help. When a screening questionnaire is a standard part of every visit, it sends a powerful message: your mental health is a key part of your overall health.
Implementing these tools delivers practical advantages:
Objective Data for Action: Screenings provide quantifiable data to track symptoms, gauge treatment effectiveness, and support clinical decisions with evidence.
Improved Efficiency: They allow busy clinics to assess many patients quickly, directing clinical resources to those who need them most. For instance, a pediatric clinic can use a waiting room tablet for parents to complete the PSC (Pediatric Symptom Checklist) for their child, flagging concerns before the appointment even begins.
Reduced Long-Term Costs: Catching issues early prevents the need for more intensive and costly treatments like emergency room visits or hospitalizations.
By learning to choose and implement the right tools, you can build a more responsive and effective practice. For more in-depth guidance on finding solutions that fit your clinic's specific needs, our team is ready to help you explore solutions via our website or email.
Navigating the Different Types of Screening Tools
Stepping into the world of mental health screening tools can feel overwhelming, but it becomes clearer when you understand the basic categories. The most effective approach is to start broad and then narrow your focus, allowing you to build a complete picture of a person's wellbeing efficiently and respectfully. You cast a wide net with general tools and only bring in more specific ones if the results indicate a potential concern.
Broad-Based General Screeners
Think of these as your first line of inquiry. General screeners quickly check for common symptoms of widespread conditions like depression and anxiety. They are the workhorses of screening in busy primary care, pediatric, and general practice settings.
Two practical examples you'll see everywhere are:
PHQ-9 (Patient Health Questionnaire-9): A nine-question tool focusing on depressive symptoms over the past two weeks. A family doctor can use this during an annual physical to quickly gauge an adult’s mood. A high score is an actionable signal to initiate a deeper conversation about mental health.
GAD-7 (Generalized Anxiety Disorder-7): A similar seven-question tool assessing the severity of anxiety symptoms. It’s a fast, effective way to flag individuals struggling with persistent worry, nervousness, or an inability to relax, prompting a discussion about anxiety management strategies.
These tools are invaluable because they are quick, easy to use, and provide a standardized score you can track over time.
Specific or Condition-Focused Screeners
If a broad-based screener raises a red flag, or if a patient presents with specific concerns, your next action is to use a more targeted tool. These instruments are designed to probe for symptoms of a single condition in greater detail.
For example, if a veteran reports poor sleep and flashbacks during a general check-in, you could administer the PCL-5 (PTSD Checklist for DSM-5). This screener is tailored specifically to the symptoms of Post-Traumatic Stress Disorder. Similarly, if substance use is a concern, a tool like the CAGE Questionnaire or AUDIT (Alcohol Use Disorders Identification Test) provides a focused inquiry. These tools help you move from a general concern to a specific area of risk, guiding your next clinical steps.
A critical insight: screening tools indicate risk; they do not confirm a condition. A high score on the PHQ-9 suggests a high likelihood of depression, but your next action is to conduct a formal diagnostic assessment to make a definitive diagnosis.
Self-Report vs. Clinician-Administered Tools
Another key distinction is who completes the assessment. This choice impacts both the patient's experience and the information you gather.
Self-Report Questionnaires: Completed directly by the patient or their caregiver (e.g., PHQ-9, GAD-7). This approach empowers patients and is incredibly efficient for busy clinics. Actionable Tip: Use tablets in the waiting room to have patients complete these before their appointment to streamline the process.
Clinician-Administered Interviews: A structured interview led by a healthcare provider. This format allows you to observe non-verbal cues and ask clarifying questions for deeper context, but it requires more dedicated clinician time.
To help you see how these tools fit into practice, the table below offers a quick comparison. For a closer look at similar assessments focused on cognition, our guide on choosing a cognitive screening test online offers further insights.
Comparison of Common Mental Health Screening Tools
Tool Name | Primary Target | Measures | Administration Format |
|---|---|---|---|
PHQ-9 | Depression | Symptoms and severity of depression | Self-Report |
GAD-7 | Anxiety | Symptoms and severity of generalized anxiety | Self-Report |
PCL-5 | PTSD | Symptoms of Post-Traumatic Stress Disorder | Self-Report |
AUDIT | Alcohol Use | Harmful alcohol consumption patterns | Self-Report or Interview |
PSC | General (Pediatric) | Broad emotional and behavioural problems in children | Self-Report (Parent/Youth) |
This comparison highlights how different tools are designed for specific purposes, helping you select the most appropriate option for your setting and population.
How to Choose the Right Tool for Your Practice
Picking the right mental health screening tool is like choosing the right lab test—precision and context are everything. The challenge isn’t finding a tool; it's finding the right one for your specific patients and clinical setting. A random choice can lead to unreliable results, wasted time, and missed opportunities to help.
You need a clear framework for this decision, moving beyond just knowing names of screeners to vetting them yourself. This ensures what you choose is clinically sound and practical for your daily workflow.
Foundational Clinical Criteria
Before considering logistics, any tool must meet non-negotiable clinical standards: validity, reliability, and cultural appropriateness.
Validity: Does this tool actually measure what it claims to? For example, a valid depression screener must accurately identify depressive symptoms, not just general stress.
Reliability: Is it consistent? If a patient's symptoms are unchanged, their score should be nearly identical a week later. Unreliable tools make it impossible to track progress.
Cultural Appropriateness: Mental health is understood differently across cultures. A tool designed for one group may not work for another. Practical example: Questions about guilt can be interpreted differently across cultures, leading to flawed results. Ensure the tool has been validated for the communities you serve.
This guide can simplify your selection process, helping you move from a broad need to a specific, well-chosen tool.
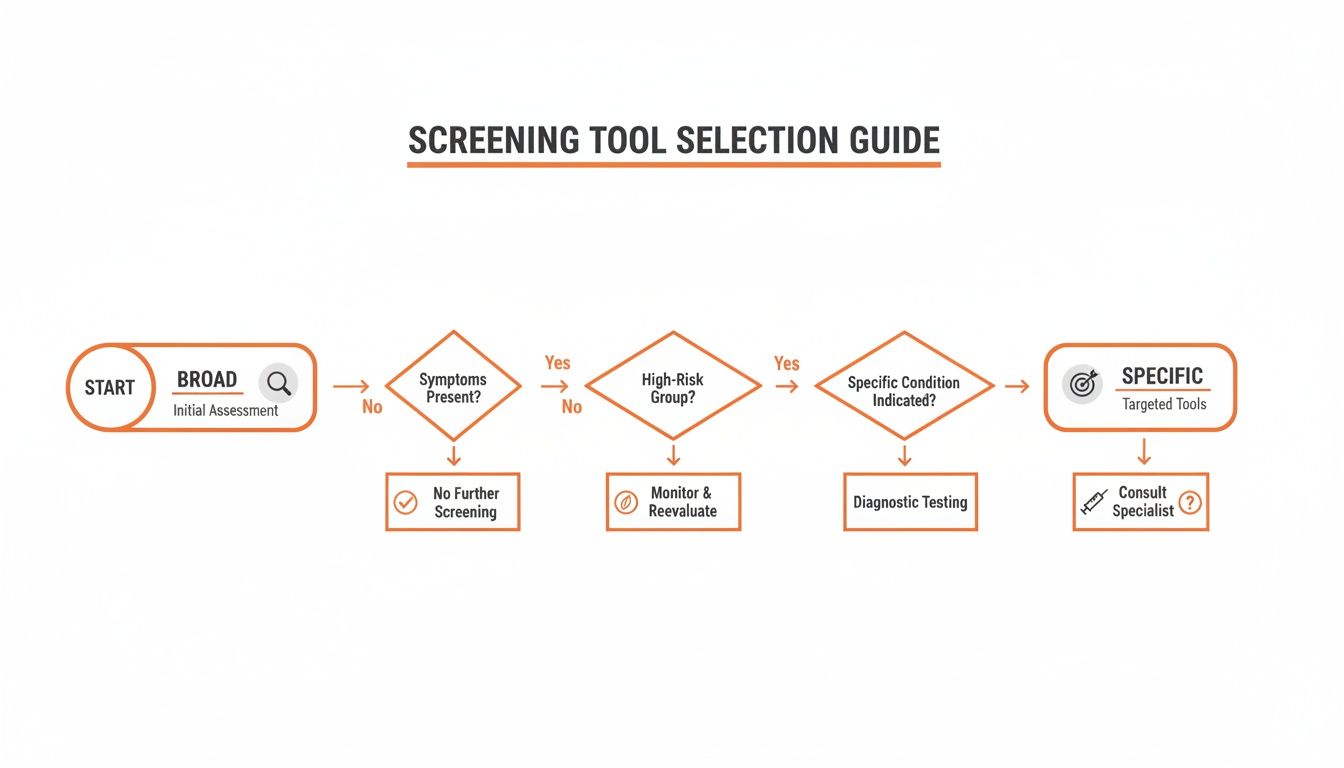
The flowchart maps out a logical path: start by defining your screening goal, narrow down by patient group and suspected condition, and land on a targeted tool that fits the situation.
Practical and Operational Factors
Once you have a shortlist of clinically sound tools, it's time to get practical. A tool that looks perfect on paper is useless if it disrupts your clinic's workflow.
The best mental health screening tool is one that gets used consistently. It must fit your patients, your staff, and your clinic's operational realities.
Here are actionable questions to ask:
Administration Time: How long does it take to complete? A 5-minute screener like the GAD-7 is feasible in a busy waiting room; a 20-minute tool is likely not.
Scoring Ease: Can it be scored instantly, or does it require special training? Actionable insight: Prioritize tools with automated digital scoring to reduce admin work and human error.
Cost and Licensing: Is it free, or does it have per-use fees or an annual license? This must fit your budget. The PHQ-9 is free, but many specialized tools are not.
EHR Integration: Does it integrate with your Electronic Health Record (EHR) system? Seamless integration means scores are automatically added to the patient’s chart, simplifying progress tracking.
For a closer look at how different assessments compare, our article exploring the MoCA vs MMSE offers more insight into how various tools are built for distinct clinical jobs. By balancing clinical rigor with practical usability, you can confidently pick an instrument that truly improves care without creating a logistical nightmare.
Weaving Screening Into Your Clinical Workflow
A mental health screening tool is only as good as its implementation. Even the best questionnaire is useless if it's not used consistently or if it creates chaos. The secret is to thoughtfully weave the tool into your existing process so it feels like a seamless, natural part of patient care.

The goal is to make screening a routine step. This normalizes the conversation around mental health and gives you consistent, objective data to back up your clinical decisions. A clear game plan helps you sidestep common hurdles like staff burnout and tight schedules.
Creating a Practical Screening Blueprint
Success starts with a simple, flexible blueprint. Instead of overhauling your entire workflow, find natural entry points to introduce a screener with minimal friction.
Here are practical examples for different settings:
Primary Care Clinic: Set up tablets in the waiting room. As patients check in, they complete a quick screener like the PHQ-9 or GAD-7. The results are scored automatically and ready in the EHR before the clinician enters the exam room.
Pediatric Office: During a well-child visit, have a medical assistant give a parent a tablet with the Pediatric Symptom Checklist (PSC). This provides a valuable snapshot of the child’s emotional health alongside their physical growth charts.
Geriatric Care: A nurse can administer a tool like the Geriatric Depression Scale (GDS) during intake. This creates a natural opening to discuss mood and memory, which are critical for this population.
This need is urgent. For example, recent data shows 94% of youth in California report mental health struggles, and over a third who wanted help were stopped by embarrassment. This is precisely why objective, low-stigma mental health screening tools are so essential.
Getting Past the Common Implementation Hurdles
The two biggest obstacles are time constraints and staff readiness. Tackle these head-on for a smooth rollout.
Here’s your action plan:
Automate Everything You Can: Use digital tools that offer automatic scoring and EHR integration. This eliminates manual data entry and frees up clinician time for patient interaction. For ideas, explore guides on implementing chatbots in healthcare to automate initial patient touchpoints.
Provide Clear, Purpose-Driven Training: Your entire team must understand the why behind screening, not just the how. Train them on introducing the tools, answering patient questions, and, most importantly, the protocol for a positive screen.
Start Small and Build Momentum: Don't try to screen every patient from day one. Actionable insight: Pilot the program with a specific group, like adults during annual physicals. Refine the process, then expand as your team gains confidence.
The most important part of your workflow isn't just identifying risk—it's responding to it. An effective program requires a clear plan for follow-up and referral, often called a "warm handoff."
The Warm Handoff Protocol
A "warm handoff" is your action plan for a positive screen. It ensures that identifying a risk immediately leads to a supportive, concrete next step, so patients don't feel flagged and abandoned.
A solid warm handoff protocol includes:
Scripted Conversation Starters: Give clinicians empathetic, non-judgmental language. For example: "Thank you for sharing this. The questionnaire picked up on some struggles with your mood. I'd like to talk more about that if you're comfortable."
Defined Next Steps: The next action must be clear. Based on the score, is a follow-up scheduled? Are educational resources provided? Or is an immediate referral to a specialist initiated?
A Curated Referral Network: Maintain an up-to-date list of trusted local therapists, psychiatrists, and support groups. Ensure your staff knows exactly how to connect patients with these resources.
By building these strategies into your practice, you transform mental health screening tools from a checklist into a powerful system for improving lives. Learn more about how Orange Neurosciences supports streamlined workflows for healthcare providers on our website or by contacting us.
Moving From Screening to Meaningful Action
Spotting a patient at risk is just the beginning. The true test of a screening program is what you do next. A program without a clear follow-up plan is like a smoke detector without a fire extinguisher—it identifies a problem but offers no solution. The real value is unlocked when a positive screen triggers a supportive and meaningful response.
Building a Robust Follow-up Protocol
Your follow-up protocol is the engine of your screening program. It ensures no at-risk patient slips through the cracks. It doesn't need to be complex, but it must be clear and consistent.
This is becoming the new standard. For example, California's Department of Health Care Services (DHCS) now requires documented follow-up care within 30 days for Medi-Cal members who screen positive for depression. This sends a powerful message: screening and action are inseparable. Learn more about these new accountability measures in California's behavioral health system.
Your protocol should outline clear actions based on scores:
Low-Risk Scores: Acknowledge the result and offer general wellness resources. This normalizes the process.
Mild to Moderate Scores: This is your cue for a brief, empathetic conversation. Actionable step: Schedule a dedicated follow-up or a re-screen in a few weeks.
High-Risk Scores: This demands immediate action. Your protocol should define how to make a warm handoff to a mental health specialist, provide crisis resources, or implement a safety plan.
Training Staff for Empathetic Conversations
Technology can't replicate human empathy. Your entire team needs training to discuss results with sensitivity. A positive screen can make a patient feel vulnerable, and a clumsy conversation can do more harm than good.
The goal is to create a safe space where patients feel heard, not judged. The conversation should be an invitation to share more.
Provide your staff with simple, scripted prompts. Instead of saying, "Your depression score is high," an actionable alternative is, "Thank you for filling this out. It looks like you've been dealing with a lot. Would you be open to talking more about what's been on your mind?" This small shift makes all the difference.
Leveraging Integrated Care and Technology
An efficient referral network is crucial. Actively build relationships with local therapists and community programs. The gold standard is an integrated care model where mental health professionals are embedded within your primary care setting.
Technology can be a powerful ally. Here's how to take action:
Automate Reminders: Set up alerts for clinicians to follow up on positive screens or for patients to complete re-assessments.
Track Patient Progress: Monitor scores over time to see if interventions are working. This objective data is priceless.
Facilitate Referrals: Use digital referral platforms to send patient information securely and track outcomes. This ensures true continuity of care.
By shifting from simple screening to meaningful action, you ensure your mental health screening tools fulfill their purpose. Discover how Orange Neurosciences can help you build this system by contacting our team today via our website or email.
Enhancing Screening with Cognitive Assessment
Most mental health screening tools tell you what—whether a patient shows signs of depression or anxiety. But what if you could also understand the why? This is where cognitive assessment comes in, offering a deeper level of patient insight.

Adding cognitive assessment doesn't replace traditional screeners; it complements them. It helps reveal the underlying brain functions contributing to mental health symptoms, moving you from identifying a problem to understanding its roots.
Pinpointing the 'Why' Behind the 'What'
Here's a practical example: a patient's PHQ-9 results show clear signs of depression. But what's driving them? A cognitive assessment might reveal that this patient also has significant deficits in executive functions like planning and decision-making.
This extra layer of objective data is an incredibly powerful, actionable insight. You're no longer just looking at a diagnosis; you're seeing the specific cognitive challenges fueling it. This allows you to build a much more targeted and effective treatment plan.
Cognitive assessment gives you a deeper, more objective dataset. It provides a window into core processing abilities—like memory, attention, and processing speed—that can directly impact a patient's mental state, enabling truly personalized care.
This principle applies across many conditions. For instance, cognitive tools are crucial for evaluating concussions. A specialized concussion baseline screening provides a critical benchmark to measure cognitive function and track recovery.
From Simple Screening to Comprehensive Brain Health
Integrating AI-powered cognitive assessments marks a shift from simple symptom spotting to a complete view of brain health. While many clinics use mental health screening tools, significant gaps often remain in making that screening actionable.
Consider this: California's 2019 perinatal mental health screening mandate led to a 25-fold rise in screenings—a huge win. Yet, by 2023, 43% of patients still had incomplete screening documentation. This highlights the gap between identifying a problem and ensuring follow-through. Cognitive tools help close that gap by providing deeper insights that justify and direct the next steps.
This level of detail makes your interventions more precise and measurable. Understanding a patient’s unique cognitive profile helps you create a care plan that addresses their specific, underlying needs. You can learn more about how Orange Neurosciences' cognitive assessments provide this detailed insight.
Ready to see how this works in practice? Reach out to us. We can show you how our AI-powered platform elevates your clinical practice from standard screening to comprehensive brain health management.
What’s the Difference Between a Screening and a Diagnosis?
This is the most important distinction. A mental health screening tool is a quick vital signs check for emotional well-being, designed to flag a potential risk.
Screening: A fast, standardized way to see if someone might have a condition, using tools like the PHQ-9 or GAD-7. A high score is an actionable signal that a closer look is warranted.
Diagnosis: A comprehensive evaluation by a qualified mental health professional, involving clinical interviews, history review, and checking symptoms against criteria (like the DSM-5) to formally identify a disorder.
A screening says, "There might be smoke here," while a diagnosis confirms, "This is the fire, and here's what kind it is."
How Should We Handle Patient Hesitation or Privacy Concerns?
It’s common for patients to be hesitant due to stigma or privacy worries. The best action is to be proactive, transparent, and empathetic.
Before handing them a form, explain the why. For example: "As part of our commitment to your whole health, we check in with all our patients about common issues like stress and mood. Your answers are completely confidential and help us provide the best care."
Framing screening as a routine part of care—like a blood pressure check—normalizes it and helps people feel less singled out. Reassure them that this information is protected just like any other part of their medical record.
Can These Screening Tools Connect with Our EHR System?
Yes. Most modern screening tools are designed for seamless integration with Electronic Health Record (EHR) systems. This is a crucial feature to look for.
When integrated, scores are sent directly to the patient's chart. This saves administrative time and eliminates manual data-entry errors. The actionable benefit is that it simplifies tracking symptom changes over time to see if a treatment is working.
While traditional screening tools are great for identifying symptoms, Orange Neurosciences helps you understand the why—the underlying cognitive functions that drive them. Our AI-powered assessments give you objective data on memory, attention, and executive function. This adds a much deeper layer of insight, helping you deliver truly personalized care.
See the whole picture of brain health. Visit us at https://orangeneurosciences.ca or contact us by email to learn more.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


