Sleep After Concussion Your Complete Guide to Rest and Recovery
Jan 18, 2026

Yes, it is absolutely safe to sleep after a concussion, as long as the injured person isn't showing severe red flag symptoms like repeated vomiting, seizures, or a headache that keeps getting worse. The old advice to keep someone awake all night is outdated. In fact, current medical guidance emphasizes that rest is essential for brain healing, especially in the first 24-48 hours.
Understanding Sleep and Safety in the First 24 Hours
The moments after a head injury can be filled with confusion and worry. One of the most persistent myths is that you have to keep someone with a concussion from falling asleep, fearing they might slip into a coma. But we now know that's not the case. Modern medicine shows that rest is precisely what an injured brain needs to start recovering.
Think of the brain after a concussion like a sprained ankle. You wouldn't force yourself to run on a swollen, painful joint, would you? You’d rest it, ice it, and give the tissues time to heal. A concussion is an injury to the brain, and sleep is the body's primary mechanism for repair.
This doesn't mean you can just leave the person completely unattended, though. The key is to practice what we call "responsible rest." This approach perfectly balances the brain's critical need for sleep with the necessity of monitoring for any signs that the injury might be more severe than it first appeared.
The Role of Monitoring and When to Worry
During the first 24 to 48 hours, a caregiver should gently wake the injured person every few hours. This doesn't mean keeping them up all night—just rousing them enough to make sure they are coherent and responsive.
Let's take a practical example: If your child gets a concussion during an afternoon soccer game, you can let them go to bed at their normal time. Just set an alarm for yourself to check on them every 2-3 hours. When you go in, gently shake their shoulder and ask a simple question like, "What's your name?" or "Where are you?" Once they respond clearly, you can let them go right back to sleep. This simple check-in helps you confirm that their condition isn't getting worse. The goal is to spot any "red flag" symptoms that could indicate something more serious is happening, like bleeding or swelling in the brain.
To make this easier, we've put together a quick-reference table. It helps you distinguish between what's normal to see after a concussion and what warrants an immediate trip to the emergency room.
Post-Concussion Monitoring Checklist for the First 24-48 Hours
Symptom to Monitor | Normal or Expected Sign | Red Flag That Needs Immediate Medical Care |
|---|---|---|
Headache | A mild to moderate headache that improves with rest or Tylenol. | A severe or worsening headache, or a "thunderclap" headache. |
Nausea/Vomiting | Mild nausea or vomiting once right after the injury. | Repeated vomiting or forceful, projectile vomiting. |
Alertness | Drowsiness, feeling "foggy," or sleeping more than usual. | Difficulty waking up, extreme drowsiness, or loss of consciousness. |
Speech | May be slightly slower or have minor trouble finding words. | Slurred speech, confusion, or nonsensical talk. |
Physical Coordination | Dizziness or slight balance issues. | Seizures, convulsions, weakness on one side, or numbness. |
Behaviour | Irritability or feeling more emotional than usual. | Unusual or bizarre behaviour, extreme agitation, or restlessness. |
Pupils | Pupils are the same size and react to light. | One pupil is larger than the other, or pupils are unresponsive to light. |
This checklist isn't exhaustive, but it covers the most critical signs. When in doubt, always err on the side of caution and seek medical help.
The flowchart below is another great tool. It provides a simple decision-making guide to help you figure out when it's safe to rest versus when you need to see a doctor right away.
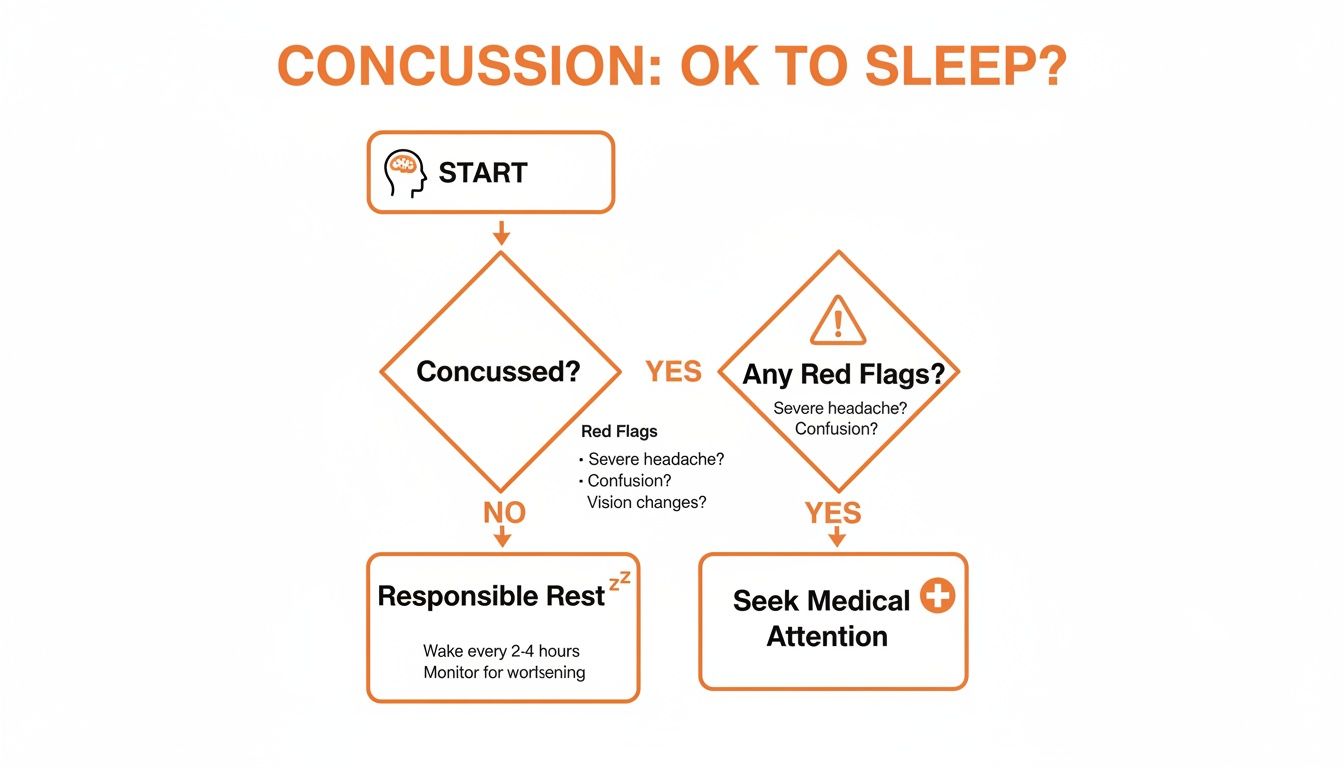
As you can see, if no red flags are present, responsible rest is the right—and necessary—path forward for recovery.
The Science Behind Why Sleep Is Crucial
Sleep isn't just a passive state of rest; it's an active period of intense neurological housekeeping. During deep sleep, the brain's glymphatic system—its unique waste-clearance network—kicks into high gear, flushing out toxins and metabolic by-products that build up while we're awake. After a concussion, this cleanup process is more important than ever. The injury creates a mess of cellular debris and inflammation that absolutely must be cleared for healing to happen.
By allowing for proper sleep, you are essentially giving the brain the time and resources it needs to run its own highly effective cleanup crew, accelerating the healing process from the inside out.
Interrupting this critical cycle by forcing someone to stay awake can actually slow down recovery and make symptoms like headaches and cognitive fog even worse.
Understanding the balance between rest and observation is the first and most important step. To dive deeper, check out our comprehensive guide on the relationship between concussion and sleep. At Orange Neurosciences, our tools can help you and your healthcare provider track cognitive recovery with objective data as you navigate the healing journey.
Why Sleep Is So Difficult After a Concussion
You've made it through the first 24 hours. The initial shock and uncertainty have passed, and you might think sleep would be a welcome relief. But for so many people, this is where a new, deeply frustrating challenge begins. If you're finding it impossible to get a good night's rest after a concussion, you're not just overtired—it's a direct consequence of the injury itself.
Think of your brain's sleep-wake cycle as a highly sophisticated air traffic control tower, expertly managing all the comings and goings. A concussion acts like a sudden, jarring power surge that throws the entire system into chaos. The delicate mechanisms that tell you when to feel sleepy and when to feel alert are knocked completely offline. This isn't just a feeling; it's a real physiological event. The injury messes with your neurotransmitters—the chemical messengers running the show—and can disrupt the production of hormones like melatonin, which is your body's natural "time for bed" signal.
The Brain's Sleep System on Overload
When your brain's sleep regulation is compromised, it struggles to do its most basic jobs. This neurological disruption shows up in several common ways, creating a confusing and exhausting experience for anyone trying to recover.
Take a student-athlete who never had trouble sleeping before their injury. Suddenly, they're staring at the ceiling for hours, their mind racing even though their body is bone-tired. This is a classic case of post-traumatic insomnia. But it can also go the other way. That same athlete might feel an overwhelming need to sleep all the time, struggling to keep their eyes open in class or during a conversation. This is hypersomnia, and it happens because the brain is pouring immense energy into healing itself, pulling resources away from things like staying awake.
These sleep-wake disturbances are incredibly common. Research from Canadian clinics paints a clear picture of just how widespread the issue is.
Data reveals that 33% of patients report sleep-wake disturbances within the first 10 days after a mild traumatic brain injury. That number jumps to 50% by six weeks post-injury. Even more telling, chronic insomnia becomes three times more common after a concussion than in the general population.
If you're struggling, know this: you are far from alone. It's a well-known part of the recovery process. You can find more insights on these findings from the Toronto Concussion Clinic.
Unpacking the Common Sleep Problems
Figuring out the specific type of sleep problem you're dealing with is the first real step toward finding a solution. While insomnia and hypersomnia are the most frequent complaints, other issues can pop up as your brain works to get back on track.
Here are the most common challenges you might be up against:
Insomnia: This isn't just one thing. It can be sleep-onset insomnia (trouble falling asleep in the first place) or sleep-maintenance insomnia (waking up constantly and struggling to get back to sleep). Headaches, anxiety, or physical pain from the injury often pour fuel on this fire.
Hypersomnia: This is that unshakable, excessive daytime sleepiness. Your brain is demanding a massive amount of energy to repair itself, leaving you in a constant state of fatigue.
Disrupted Sleep-Wake Cycle: Your internal body clock, or circadian rhythm, can be thrown completely haywire. You might find yourself wide awake at 3 a.m. but desperately needing a nap by mid-afternoon. It makes sticking to any kind of routine—for school, work, or life—feel impossible.
Poor Sleep Quality: You might be in bed for eight hours but wake up feeling like you haven't slept at all. A concussion can rob you of deep, restorative sleep stages, which are absolutely essential for both physical and cognitive healing.
By identifying which of these patterns fits your experience, you can have a much more productive conversation with your doctor or therapist. This clarity is key to moving from just coping with bad sleep to actively treating it. At Orange Neurosciences, our tools are designed to help you and your clinician track the cognitive changes that go hand-in-hand with sleep disruption, providing objective data to guide your healing journey. For more information, visit our website to learn how we can help.
The Hidden Risk of Too Much Sleep for Kids and Teens
When your child gets a concussion, your first instinct is probably to wrap them in a blanket and let them sleep as much as they possibly can. This comes from a place of love, but recent findings show a surprising twist in pediatric concussion care: too much sleep can actually work against recovery.
It’s a strange paradox, but understanding it is crucial for guiding your child back to health. Think of recovery like trying to balance a scale. On one side, you have the absolute need for rest, especially in those first few days. On the other, you have the need for a gradual, safe return to daily life. Tipping the scale too far in either direction can slow everything down. It turns out that excessive sleep can tip the scale too far toward inactivity, getting in the way of the brain's natural ability to recalibrate.
This isn’t just a theory; it’s backed by important Canadian research. Finding that 'sweet spot' for rest is one of the most proactive steps you can take.

Why More Isn't Always Better
A young, developing brain thrives on routine. When a child or teen sleeps way too much for days or weeks, it throws their natural circadian rhythm—the body's internal clock—completely out of whack. This can kickstart a frustrating cycle where they feel groggy and exhausted during the day, which only makes other concussion symptoms like headaches and irritability even worse.
A landmark Ontario cohort study from the Pediatric Concussion Assessment of Rest and Exertion (PedCARE) gave us clear data on this. The study looked at 291 adolescents and found a direct link between how long they slept and how severe their symptoms were. It showed that sleeping more than 9.5 hours in the first week or 9.9 hours over two weeks was connected to a higher symptom burden. This actually increased the risk of symptoms sticking around for more than a month. This means that while rest is absolutely non-negotiable, a strategy of unlimited sleep can backfire.
The key takeaway for parents is that after the first few days of acute recovery, the focus should shift from 'maximum rest' to 'optimal rest.' This means encouraging a consistent sleep schedule that supports healing without promoting inactivity.
Finding the Sweet Spot: A Practical Example
So, what does this actually look like? Imagine your 14-year-old daughter gets a concussion at soccer practice. Here’s a step-by-step action plan to manage her sleep for a balanced recovery:
Days 1-3 (The Acute Phase): Let her sleep as much as she needs. Her brain is in emergency repair mode. You’ll still monitor her for any warning signs, but the priority is deep, uninterrupted rest.
Days 4-7 (The Transition): Now, you can start reintroducing a gentle structure. Encourage her to get up at a consistent time, even if she still feels tired. A short, 20-30 minute nap in the early afternoon is perfectly fine, but try to avoid long, unstructured daytime snoozes that will mess with her nighttime sleep.
Week 2 and Beyond (The Structured Phase): Work towards a firm bedtime and wake-up time. Aim for about 9-10 hours of sleep a night, which is right for her age. This regularity helps reset her internal clock and seriously improves her sleep quality.
This gradual shift helps the brain move from a passive state of healing to an active one, which is vital for rebuilding those important neural connections.
For more personalized support, our resources for parents and individuals can offer guidance on managing these recovery milestones.
Using Tools to Track Progress
One of the toughest challenges for parents is figuring out if your strategy is working. Is your child's lingering fatigue a sign they need more rest, or a sign that too much rest is becoming the problem? This is where having some objective data can be a total game-changer. Cognitive tracking tools, like those we offer at Orange Neurosciences, provide a clear window into your child's brain function. By measuring things like attention and processing speed over time, you and your doctor can see exactly how recovery is progressing.
If cognitive scores stall or even dip alongside a pattern of excessive sleep, it provides strong, data-driven evidence that it's time to adjust the recovery plan. This lets you move beyond guesswork and take an informed, proactive role in your child’s healing journey.
Actionable Strategies to Improve Your Sleep Hygiene
Getting a grip on your sleep is one of the most powerful things you can do for your concussion recovery. While your brain is healing, it becomes incredibly sensitive to the world around it. The usual tricks for sleeplessness might not work—in fact, they could even cause overstimulation and make your symptoms worse.
This is your practical toolkit. It’s about building healthy sleep habits that respect what your brain is going through right now. Think of your bedroom as a recovery sanctuary. After a concussion, it's extremely common to be sensitive to light and sound, which can make falling asleep feel like an impossible task. The goal here is to dial down the sensory input and create a 'brain-friendly' environment that clearly signals it's time to rest.

Create a Brain-Friendly Sleep Sanctuary
First things first: manage your environment. Your brain is already working overtime to heal, so cutting down its workload at night is a non-negotiable for quality sleep. Here's your action plan:
Darkness is Your Ally: Use blackout curtains or a good eye mask to get your room as dark as possible. Even tiny amounts of light from electronics or streetlamps can mess with the production of melatonin, your body's natural sleep hormone.
Silence the Noise: If sounds are bothering you, earplugs are a simple but game-changing solution. A white noise machine can also work wonders by masking disruptive sounds with a steady, soothing backdrop.
Keep It Cool: A cooler room temperature is a key signal to your body that it's time to sleep. Aim for a temperature that feels comfortable but slightly cool, usually somewhere between 15-19°C (60-67°F).
For example, someone recovering from a concussion might find the glowing numbers on their alarm clock painfully bright. A small change, like switching to a clock with a dimmable display or just turning it away from the bed, can remove that source of visual static and make it much easier for a sensitive brain to relax.
Establish a Calming Wind-Down Routine
A consistent evening routine is like a gentle off-ramp for your brain. It helps you transition smoothly from the buzz of the day into a state of rest. This is especially important after a concussion when you're more prone to overstimulation. The key is to make it calming and predictable.
A wind-down routine doesn't need to be complex. The real goal is consistency. When you do the same quiet things in the same order every night, you're teaching your brain to associate those activities with sleep.
Start this routine about 30-60 minutes before you want to be asleep. Choose activities that are low-stimulation and won't trigger symptoms like headaches or dizziness.
Dim the Lights: About an hour before bed, lower the lights in your home to signal that the day is ending.
Unplug from Screens: The blue light from phones, tablets, and computers is a major disruptor to your sleep cycle. Put them away at least an hour before you turn in.
Engage in Quiet Activities: Try reading a physical book (not on a bright screen), listening to calm music or a podcast at a low volume, or doing some gentle stretching.
This is particularly critical for young people. In Canada, concussions affect over 100,000 children and adolescents every year, and sleep disruption is one of the biggest roadblocks to their healing. One major study found that insomnia affected two-thirds of adolescents who were slow to recover from a concussion. When they received targeted therapy to improve their sleep, they not only healed faster but also had fewer doctor visits, and their parents missed less work. It's a powerful reminder of how vital a consistent schedule is.
Manage Light Exposure and Screen Time
Light is the single most powerful cue for your body's internal clock. Getting your light exposure right is absolutely fundamental to improving sleep after a concussion.
Your strategy should be simple: get bright light during the day and avoid it at night. Stepping outside for just 10-15 minutes of sunlight first thing in the morning can help lock in your body's clock, making you feel more alert during the day and sleepy at night.
On the flip side, screen time in the evening is a major problem. The blue light from our devices tricks the brain into thinking it's still daytime, which suppresses melatonin and makes it much harder to fall asleep. If you absolutely can't avoid screens, try using blue-light-filtering glasses or turn on your device's "night mode" setting in the evening.
For anyone looking for more structured support on their recovery journey, professional neurorehabilitation programs can offer a guided path to restoring healthy sleep patterns and cognitive function. And for some general, drug-free strategies that can help anyone, you might find these five tips for falling asleep quicker useful, too. Taking these small, practical steps can make a huge difference, putting you back in the driver's seat of your own healing process.
When to Seek Professional Help for Sleep Issues
Improving your sleep hygiene is a huge first step, but sometimes, lifestyle tweaks alone aren't enough to get your sleep cycle back on solid ground. A recovering brain is a sensitive one, and persistent sleep problems can seriously pump the brakes on your healing. Knowing when to shift from self-management to professional guidance is a crucial part of a successful recovery.
Think of it this way: good sleep hygiene is like doing regular maintenance on your car. It keeps things running smoothly most of the time. But when a warning light stays on no matter what you do, you need a mechanic to diagnose the real problem. Lingering sleep issues after a concussion are your brain’s warning light.
Recognizing the Signs It's Time for Help
If you've been diligently working on your sleep habits for a few weeks without any real improvement, it's time to talk to your doctor. Don't wait for months to pass. Poor sleep can crank up the volume on other concussion symptoms like headaches and brain fog, creating a vicious cycle that’s tough to break.
Here are some clear signs that you should book an appointment:
Persistent Insomnia: You’re consistently struggling to fall asleep or stay asleep for more than two to four weeks.
Excessive Daytime Sleepiness: You feel completely wiped out during the day, even after what felt like a full night's sleep.
Worsening Mood: Your sleep issues are fuelling more anxiety, irritability, or feelings of depression.
Impacting Daily Function: Fatigue and sleep deprivation are making it hard to keep up with work, school, or even just your basic daily routine.
When post-concussion sleep problems just won't quit, professional guidance is the next logical step. You could also look into options like working with a certified sleep coach for more structured support.
The Role of Medication and Non-Medication Therapies
When you do seek help, it’s important to have a real, informed conversation with your healthcare provider about your options. Treatment isn't just about popping a pill; in fact, non-drug therapies are often the first and most effective line of defence for post-concussion sleep problems.
Medication: A brain healing from an injury is incredibly sensitive, so medications must be used with extreme caution and only under a doctor's supervision.
Melatonin: It might be available over-the-counter, but the timing and dosage are everything. Using it incorrectly can actually throw your body clock off even more.
Prescription Medications: Your doctor might consider certain antidepressants or specific sleep aids, but they'll need to carefully weigh the benefits against potential side effects, like next-day grogginess that could get in the way of your cognitive recovery.
Non-Medication Therapies: These approaches are designed to fix the root cause of the sleep problem, not just put a bandage on the symptoms.
The gold standard for treating chronic insomnia is a powerful, non-medication treatment called Cognitive Behavioural Therapy for Insomnia (CBT-I). This therapy helps you identify and rewire the thoughts and behaviours that are keeping you awake.
For example, a key part of CBT-I is something called stimulus control. If you’ve started to associate your bed with tossing, turning, and frustration, a therapist might tell you to get out of bed if you aren't asleep within 20 minutes. You’d go to another room and do something quiet and relaxing until you feel sleepy again. This process retrains your brain to see your bed as a place for sleep, not a battleground.
How Objective Data Can Guide Your Treatment
It's one thing to tell your doctor, "I'm not sleeping well." It's another thing entirely to walk in with hard data. Having a productive conversation with a sleep specialist or neuropsychologist is so much easier when you come prepared.
This is where having objective data can make a world of difference. By tracking your cognitive function over time, you can show your doctor concrete evidence of how poor sleep is impacting your attention, memory, and processing speed. This data doesn't just support clinical decisions; it helps create a treatment plan that's truly tailored to you and gives you a clear way to see if it's actually working. For a deeper dive into managing your recovery, check out our guide to complete concussion management.
Frequently Asked Questions About Sleep and Concussions
Working through a concussion brings up a ton of questions, especially about something as fundamental as sleep. Feeling unsure about what to do is completely normal. Here, we’ll tackle some of the most common concerns we hear, giving you clear, straightforward answers to help you navigate your recovery with a bit more confidence.
How Long Will My Sleep Problems Last After a Concussion?
This is the big question on everyone's mind, and the honest answer is: it really varies. For many people, sleep starts getting back to normal within a few weeks as the brain heals. But for a lot of others, problems like insomnia can stick around for months if they aren't addressed head-on.
How long it takes depends on a few things: the severity of your injury, what your sleep was like before the concussion, and how well you're practicing good sleep habits now. If you've been consistent with good sleep hygiene for two to four weeks and you’re still struggling, that's your cue to talk to your healthcare provider for a more personalized plan.
Can I Use Over-the-Counter Sleep Aids Like Melatonin?
It’s incredibly tempting to reach for something to get a good night's rest, but you absolutely must talk to your doctor before taking any kind of sleep aid—including melatonin—after a concussion. A healing brain is far more sensitive to medications and supplements. What was perfectly safe for you before your injury might not be now.
While melatonin can be helpful for resetting your internal clock, the dosage and timing are everything. Get it wrong, and you could actually make your sleep problems worse. It's also critical to steer clear of other over-the-counter sleep aids, particularly those with sedating antihistamines, unless your doctor has specifically approved them. They can leave you feeling foggy the next day and get in the way of your cognitive recovery.
Think of it this way: you wouldn't try to adjust the fuel mixture in a high-performance engine without an expert's guidance. Your brain is far more complex. Always let a medical professional guide any chemical interventions during your recovery.
My Teenager Wants to Sleep All Day. Should I Let Them?
While extra rest is crucial in the first couple of days after the injury, letting a teenager sleep all day beyond that initial window can actually do more harm than good. This might sound surprising, but it’s a key finding in pediatric concussion care.
Canadian research has found that for adolescents, sleeping more than 9.5 to 10 hours a day in the weeks following a concussion is linked to worse symptoms and a longer recovery. Too much sleep throws their natural circadian rhythm out of whack, which can amplify headaches, fatigue, and irritability.
Instead of letting them sleep in, your actionable insight is to implement a consistent sleep schedule with a regular bedtime and wake-up time. If they're tired during the day, short, structured naps of 20 to 30 minutes are a much better strategy than long, unstructured sleep that messes with their nighttime rest.
How Does Poor Sleep Affect My Other Concussion Symptoms?
Sleep is prime time for your brain’s repair crew. When that process gets disrupted, the entire healing project slows down. Poor sleep doesn’t just make you tired; it actively makes other concussion symptoms worse.
This kicks off a frustrating and vicious cycle. For instance:
Headaches: A lack of deep, restorative sleep can make post-concussion headaches more frequent and much more intense.
Cognitive Function: Sleep deprivation is a major blow to your attention, memory, and processing speed, making that "brain fog" feel ten times thicker.
Emotional Regulation: When you're running on empty, it's so much harder to manage the irritability, anxiety, and mood swings that often come with a concussion.
The stress from these worsening symptoms then makes it even harder to fall asleep the next night. That’s why making sleep a priority isn't just a nice idea—it’s a non-negotiable part of any effective concussion recovery plan. Keeping track of how your symptoms fluctuate day-to-day can give your doctor crucial insights. You can learn more about how to identify and monitor these issues with a detailed concussion symptom questionnaire.
At Orange Neurosciences, we understand that objective data is key to a successful recovery. Our evidence-based platform provides precise cognitive assessments that help you and your clinician track progress, remove guesswork, and make better-informed decisions about your care plan. Visit us at https://orangeneurosciences.ca to see how our tools can support your journey back to brain health. To stay updated with the latest insights on brain health and recovery, subscribe to our newsletter for actionable tips delivered right to your inbox.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


