Ontario Brain Institute: A Guide for Health Innovators
Apr 15, 2026

You might be looking at the ontario brain institute because you have something promising in hand, but not yet a clear path forward.
Maybe you're a neurologist with a better way to monitor concussion recovery. Maybe you're a rehab leader trying to bring cognitive tools into routine care without creating extra work for staff. Maybe you're building an AI-enabled platform and need access to credible research networks, governed data, and the kind of collaborators who can move a pilot into real clinical use.
That’s where many people get stuck. Good ideas often fail at the same points: no shared data standard, no trusted introduction to the right hospital or research team, no practical route from prototype to evaluation, and no one coordinating the pieces across Ontario.
The ontario brain institute, usually called OBI, exists to close that gap. It helps connect research, care, data infrastructure, patient partnership, and commercialization so that brain health innovation can move with more structure and less guesswork.
Your Gateway to Brain Health Innovation in Ontario
A common Ontario story goes like this. A clinician develops a strong care idea after seeing the same problem repeatedly in practice. The idea makes sense clinically, but the next questions pile up fast. Who can help validate it? Where can you find the right patient population? How do you build evidence that another institution will trust?
OBI was built for that middle ground between idea and impact.
It was established in 2010 to address the needs of approximately 1 million Ontarians then living with brain disorders, and it has since grown into an important organization supporting patients, leveraging funding, and helping the 1 in 3 Ontarians affected by a brain disorder today, as described in the Canadian Journal of Neurological Sciences overview of OBI.
Why people turn to OBI
Most innovators don’t need just one thing. They need several things at once.
A credible network: access to researchers, clinicians, community sites, and decision-makers.
A practical research home: a place where studies, pilots, and data-sharing can fit into existing structures.
A translation pathway: support that doesn’t stop at discovery, but also considers implementation and commercialization.
If you work in digital health, this broader context matters. The policy, workflow, and deployment side of innovation often matters as much as the model itself. For extra context on these aspects, this overview of AI healthcare solutions in Canada is a useful companion read.
OBI is easiest to understand as a provincial connector. It doesn’t simply fund ideas. It helps assemble the conditions that make those ideas testable and usable.
A practical example
Say a team has built a digital cognitive assessment that produces fast profiles for attention, memory, and executive function. The tool may already be usable in practice, but the team still needs stronger external validation, collaborators across care settings, and a path into brain health networks that value standardization.
That’s the kind of setting where OBI becomes relevant. It can be a practical entry point for organizations pursuing broader digital brain health partnerships across the country, including efforts like Orange Neurosciences and the DOT Canada expanding digital brain health across Canada.
Understanding the OBI Mission and Structure
OBI makes more sense when you stop thinking of it as a single institute with one lab or one hospital base.
It operates more like an ecosystem architect. Its job is to create the structures that let many groups work together with less friction.
What OBI actually is
OBI is a provincially funded not-for-profit that uses a collaborative team science model. In plain language, that means it brings together groups that often work in parallel but need one another to create real-world change.
Those groups include:
Group | What they contribute |
|---|---|
Academic researchers | Study design, analysis, scientific depth |
Clinicians | Real care questions, patient pathways, implementation realities |
Industry partners | Product development, usability, scale |
Patients and caregivers | Lived experience, relevance, practical priorities |
Policymakers and system leaders | Alignment with provincial needs and adoption pathways |
A traditional institute may focus on producing research internally. OBI focuses on organising collaboration across the province.
Why the structure matters
Collaboration in brain health is difficult for predictable reasons.
One hospital may collect different measures than another. A startup may speak in product terms while a clinician thinks in workflow terms. A research team may want rigour, while a community partner needs a process that’s realistic for participants.
OBI’s model helps align those interests.
Practical rule: If your project depends on cross-site trust, shared standards, or multiple stakeholder groups, OBI is often more relevant than a stand-alone research partner.
That’s also why OBI is often described as an honest broker. It can support data-sharing and partnership building without forcing every participant into the same institutional box.
How to think about fit
Ask three questions.
Is your work tied to a real brain health problem in Ontario?
OBI is strongest when a project addresses a clear clinical, research, or community need.Does your work require collaboration across settings?
If you need hospitals, academic teams, community groups, or industry working together, OBI’s structure helps.Can your work benefit from common standards?
Projects involving cognitive assessment, longitudinal monitoring, neurotechnology testing, or AI validation often do.
For organizations assessing long-term fit with values, leadership, and translational focus, background on mission and orientation can help before outreach begins. A simple starting point is the Orange Neurosciences team and company overview, which shows the kind of practical platform profile collaborators often compare against OBI-linked opportunities.
Exploring OBIs Integrated Discovery Programs
The clearest way to understand OBI in practice is to look at its Integrated Discovery Programs, often shortened to IDPs.
These are province-wide research networks organised around specific brain health areas. They don’t just gather data. They create shared methods, connect institutions, and make it easier to move findings into care and innovation.
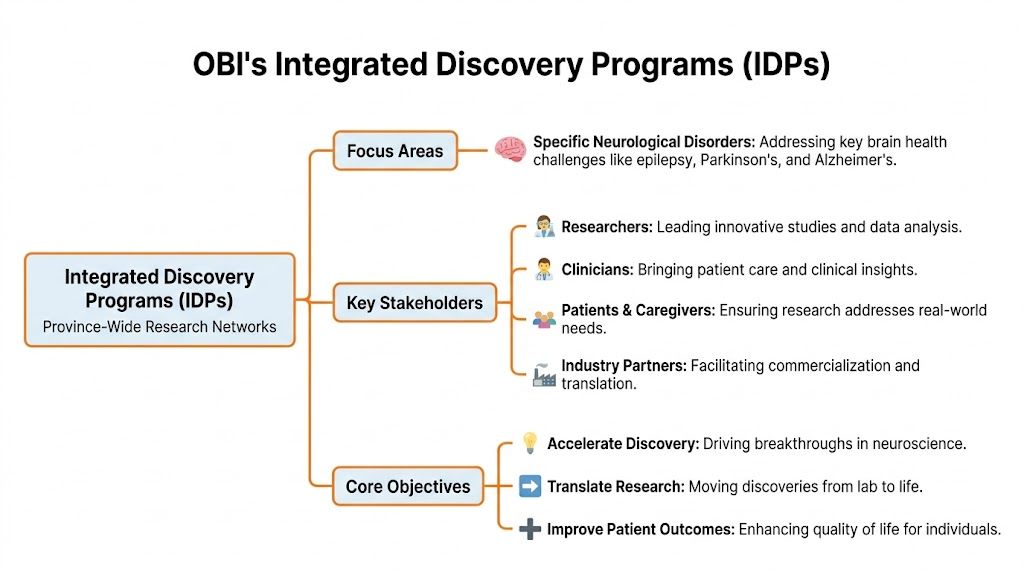
What an IDP does
An IDP usually combines several elements at once:
A defined clinical focus: such as neurodevelopmental disorders, concussion, depression, or cerebral palsy.
Shared assessments: so data from one site can be compared with data from another.
Cross-disciplinary teams: researchers, clinicians, and lived-experience partners all contribute.
Translation goals: findings are meant to support better tools, interventions, or decisions.
That combination is what makes the model practical for collaborators. You’re not entering a loose network. You’re entering a structured one.
Concrete examples that help
A few examples show how these programs work on the ground.
POND is one of the best-known examples. OBI describes how POND’s work on shared biology across disorders has identified overlapping genetic and neurodevelopmental pathways in ADHD and autism, helping move research toward more targeted interventions through biomarker-linked therapeutic response.
CONNECT is another strong example. It supports concussion research and contributes to a major pediatric concussion dataset that researchers use to build better recovery models.
Other OBI-linked programs focus on areas such as youth mental health, cerebral palsy, depression, neurodegeneration, and epilepsy. You don’t need to fit every part of your work into one program. What matters is identifying where your problem, patient group, or method already overlaps with an active network.
Where CORTEX fits
Not every innovation challenge starts in a research lab. Some begin in community care, long-term support settings, or real-world service environments where usability matters as much as scientific promise.
That’s where CORTEX is useful. OBI notes that programs like CORTEX are designed to co-design and test neurotechnologies with lived-experience partners in real-world settings, including Alzheimer Society sites, so innovations are practical and effective for community use across Ontario in this discussion of how OBI is filling gaps in brain research.
If your tool works in theory but hasn’t yet been tested in the everyday conditions of community care, a program like CORTEX is often more relevant than a purely academic study.
How to identify the right IDP
Use a matching approach instead of starting with funding.
Match by condition: concussion, neurodevelopment, depression, dementia-related care, and so on.
Match by workflow problem: screening, monitoring, recovery tracking, therapy response, community implementation.
Match by data type: behavioural, imaging, genetic, cognitive, or multimodal.
Match by deployment setting: hospital, clinic, school-linked service, rehab site, community partner.
That simple shift helps. Instead of asking, “Can OBI support my idea?” ask, “Which existing OBI structure already touches the problem I’m trying to solve?”
Accessing Data with Brain-CODE and the Centre for Analytics
For many collaborators, the most valuable part of OBI isn’t just the network. It’s the combination of Brain-CODE and the Centre for Analytics.
One gives you governed, standardised data. The other creates a pathway for advanced analysis, including AI and machine learning work.

Brain-CODE in plain language
Think of Brain-CODE as a secure neuroinformatics platform built to support sharing and analysis across OBI’s research programs.
It includes standardised, multi-modal data from over 29,555 participants across Ontario, including the world’s largest dataset on pediatric concussions, and that dataset has been downloaded over 100 times internationally, according to OBI’s summary of how Brain-CODE data is impacting healthcare worldwide.
That description can sound abstract, so here’s the practical meaning. Brain-CODE doesn’t just hold one kind of information. It supports combinations of data such as behavioural, imaging, genetic, molecular, and clinical measures, gathered in ways that make cross-site use possible.
Why standardisation matters more than size alone
A large dataset is helpful. A large dataset collected in incompatible ways is much less helpful.
Brain-CODE’s value comes from standardisation. When assessments and data structures are aligned, researchers can compare patterns across disorders, sites, and participant groups more confidently. That’s how a platform moves from being a storage system to being an engine for discovery.
This is especially relevant for cognitive technologies. If you’re trying to validate an assessment tool, benchmark a new measure, or understand how your outputs relate to broader neurological profiles, consistency matters as much as access.
A useful parallel is the importance of measurement quality in reliability work. This guide to test-retest reliability statistics is a good reminder that the usefulness of any cognitive tool depends on whether its outputs remain stable and interpretable across repeated use.
Where the Centre for Analytics comes in
The Centre for Analytics, or CfA, is the layer that helps turn harmonised data into predictive and clinically relevant models.
OBI identifies a key opportunity for AI-driven platforms in collaborating with the CfA, which was established through part of the $65M provincial funding renewal in 2024, to validate assessment tools against large-scale datasets and contribute to new predictive AI models in OBI’s funding renewal overview.
That creates a practical sequence:
Data are collected and harmonised through OBI-linked programs.
Researchers and collaborators analyse patterns across those datasets.
CfA-supported methods help build stronger prediction, stratification, or validation approaches.
Tools and insights move closer to care use, product development, or trial design.
A company doesn’t need to arrive with a finished AI solution. It needs a clear clinical use case, a defensible measurement approach, and a realistic plan for validation.
Questions to ask before pursuing data collaboration
Before reaching out, it helps to be specific.
What exactly do you want to validate? A score, a risk flag, a recovery profile, a treatment-response marker?
Which population matters most? Children, older adults, concussion patients, neurodevelopmental cohorts, community users?
What kind of access do you need? Benchmarking, retrospective analysis, algorithm development, or pilot feasibility planning?
What governance constraints apply? Institutional approval, privacy review, data minimisation, and intended use all matter.
The more concrete your answer, the easier it is for an OBI conversation to become productive.
Funding and Commercialization Pathways for Neurotech
Some organisations come to OBI for data. Others come because they need a route from early evidence to market traction.
That side of OBI matters just as much.
What commercialization support looks like
OBI’s neurotech programs, including NERVE and NERD, support a sizeable portfolio of Ontario companies. OBI reports that its programs support over 110 portfolio companies, and those companies have attracted over $440.5 million in follow-on investment, achieving a 25.9x return on OBI’s initial funding in its overview of Ontario’s role in a growing Canadian neurotech market.
That tells potential collaborators something important. OBI doesn’t treat commercialization as an afterthought. It treats it as part of the translation pathway.
A realistic startup journey
Consider a hypothetical neurotech company building a cognitive monitoring tool for rehab settings.
At the start, the team may need help refining the use case. Their first challenge isn’t scale. It’s proving that clinicians will use the tool, that the outputs mean something, and that the workflow burden stays low.
OBI-linked commercialization support can help at that stage by giving the company:
Early credibility: association with a recognised provincial brain health network.
Better introductions: access to clinicians, evaluators, and possible pilot environments.
Stronger investor readiness: clearer evidence, cleaner positioning, and more realistic adoption planning.
That last part matters. Many founders explain the science well but struggle to explain the business case. If you’re preparing for investor conversations, this guide on how to create a pitch deck that wins funding is a useful complement to the clinical side of your preparation.
Why OBI support changes the conversation
A grant alone can help you survive. A well-placed strategic partner can help you mature.
When a neurotech company works through OBI-linked channels, it’s often doing more than raising money. It’s gathering the evidence and relationships that later funders, pilot sites, and health system buyers want to see.
Investors may back a promising concept. Clinical partners usually need something more specific: evidence that the tool fits a real workflow and solves a real problem.
That’s one reason OBI-backed visibility can matter for international positioning as well as local traction. Public-facing examples of Canadian digital health participation in global forums, such as Orange Neurosciences showcasing Canadian digital health innovation at the G20 DIA in Bengaluru, show how provincial credibility can support broader market conversations.
How Your Organization Can Collaborate with OBI
A high-level summary isn’t what is needed. Instead, a starting plan is.
The practical route into OBI depends on whether you’re approaching as a researcher, clinician, or neurotech company. The steps overlap, but the preparation should be different for each.

If you’re an academic researcher
Start with alignment, not application.
Review OBI’s program areas and ask where your work already overlaps with an active network. A weak outreach message says, “I’d like to collaborate.” A stronger one says, “My team studies treatment response in youth mental health, and our methods may fit an existing OBI data or program structure.”
Then prepare a short collaboration brief with:
Your research question
Your target population
The data or network access you need
The benefit to the existing OBI ecosystem
Your institutional readiness for ethics and governance review
If your institution already works with external research platforms, mention that. It reduces uncertainty.
If you’re a frontline clinician or service leader
Lead with the care problem.
OBI-linked teams need to know what isn’t working in practice. Are diagnostic delays too long? Are community patients poorly represented in current studies? Is there a technology that could help, but staff need a realistic pilot structure?
Your strongest contribution may be a care environment, not a dataset.
A useful clinician outreach note often includes:
A defined patient group
A workflow gap
A feasible pilot setting
What support your team can provide
What would count as a successful result
That level of specificity helps OBI identify whether your idea belongs in a trial, a community implementation effort, or an evaluation partnership.
If you’re a neurotech company
At this point many questions become more technical.
The most promising route is often not “Can we plug into OBI?” but “How can our tool fit responsibly within OBI’s research and data environment?” OBI has identified collaboration with the Centre for Analytics as a key opportunity for AI-driven platforms, using part of the $65M provincial renewal in 2024 to support validation against large-scale datasets and the development of predictive AI models.
That points to a practical checklist.
Define intended use clearly: screening support, cognitive monitoring, therapy planning, reassessment, or research use.
Separate product claims from research goals: avoid overstating what the tool can do before validation.
Map your data elements: know which outputs are behavioural, performance-based, patient-reported, or metadata.
Plan for privacy compliance: if data sharing is part of the proposal, be ready to discuss governance under Ontario requirements such as PHIPA in a careful, institution-specific way.
Prepare an interoperability summary: show how results can be exported, structured, or compared without disrupting clinician workflow.
The best partnership proposals are modest, precise, and easy to evaluate. “We want to benchmark our executive function outputs against relevant OBI-linked datasets under approved protocols” is far stronger than “We want to transform brain health with AI.”
A simple engagement template
Here’s a plain-language way to structure first contact.
What to include | Why it helps |
|---|---|
One-sentence description of your organisation | Gives immediate context |
The brain health problem you address | Shows relevance |
The OBI resource you believe fits | Signals you’ve done your homework |
Your proposed next step | Makes the ask concrete |
Governance readiness | Builds trust early |
Academic groups looking for external partners can also strengthen their approach by clarifying how a tool, site, or dataset would support teaching, validation, or translational studies. This page for academic institution partnerships is a useful example of how organisations frame collaboration readiness in a way universities can assess quickly.
Building the Future of Brain Health Together
The ontario brain institute is most useful when you see it for what it is. Not a single lab. Not only a funder. Not just a data repository.
It is a coordinated brain health network built to help Ontario innovators connect research, care, data, and commercialization in a more usable way. If your organisation needs a serious path into collaboration, validation, or real-world neurotechnology deployment, OBI is a strong place to begin. Visit the OBI website, review its current programs and partnership pathways, and contact the team with a focused proposal that matches a real clinical or research need.
If your team is exploring practical digital brain health delivery in Canada, Orange Neurosciences offers an AI-powered platform for rapid cognitive assessment and targeted therapy that can support clinics, educators, researchers, and care organisations looking to build evidence-based workflows.

Orange Neurosciences' Cognitive Skills Assessments (CSA) are intended as an aid for assessing the cognitive well-being of an individual. In a clinical setting, the CSA results (when interpreted by a qualified healthcare provider) may be used as an aid in determining whether further cognitive evaluation is needed. Orange Neurosciences' brain training programs are designed to promote and encourage overall cognitive health. Orange Neurosciences does not offer any medical diagnosis or treatment of any medical disease or condition. Orange Neurosciences products may also be used for research purposes for any range of cognition-related assessments. If used for research purposes, all use of the product must comply with the appropriate human subjects' procedures as they exist within the researcher's institution and will be the researcher's responsibility. All such human subject protections shall be under the provisions of all applicable sections of the Code of Federal Regulations.
© 2026 by Orange Neurosciences Corporation


